2008 JCO Study of Orthodontic Diagnosis and Treatment Procedures, Part 2: Breakdowns of Selected Variables
Patient Demographics
Similar articles from the archive:
- 2002 JCO Study of Orthodontic Diagnosis and Treatment Procedures, Part 2: Breakdowns of Selected Variables November 2002
- 1996 JCO Study of Orthodontic Diagnosis and Treatment Procedures, Part 2: Breakdowns of Selected Variables December 1996
- 1990 JCO Study of Orthodontic Diagnosis and Treatment Procedures, Part 2: Breakdowns of Selected Variables April 1991
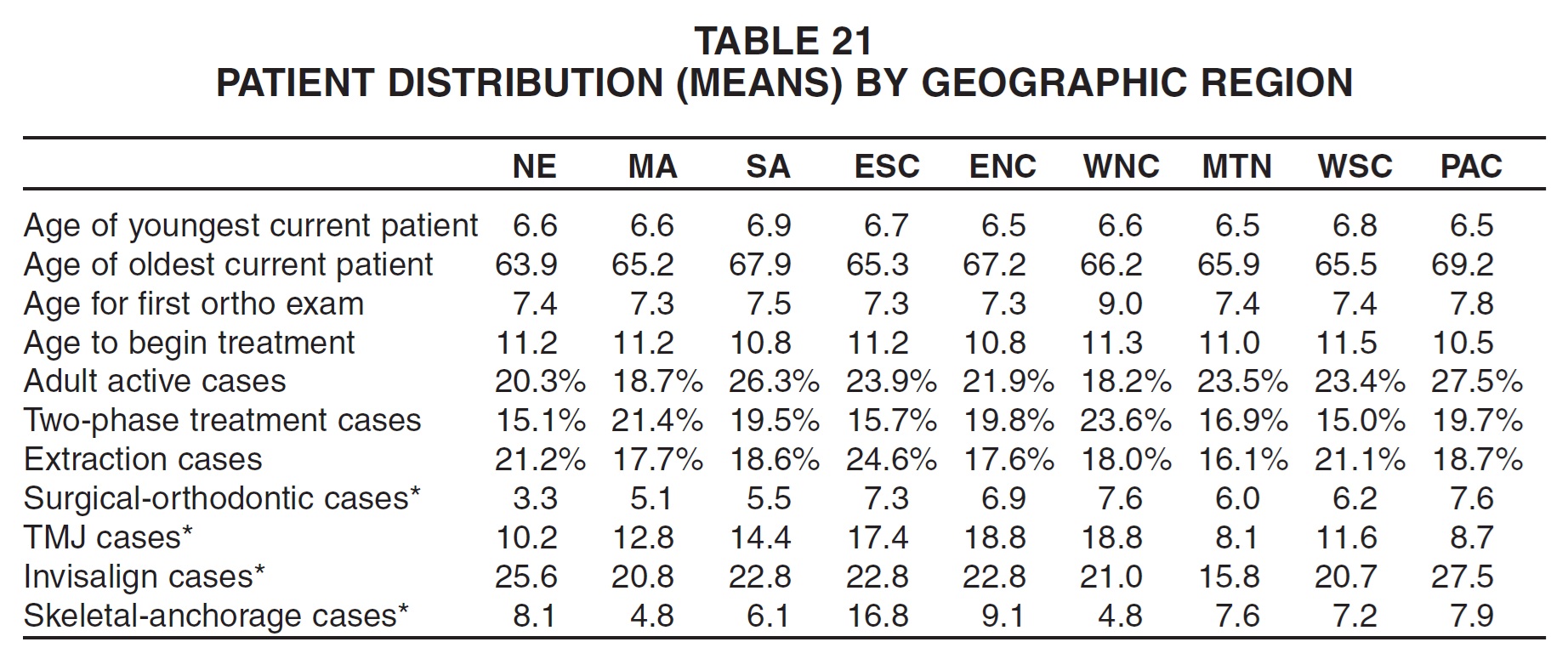
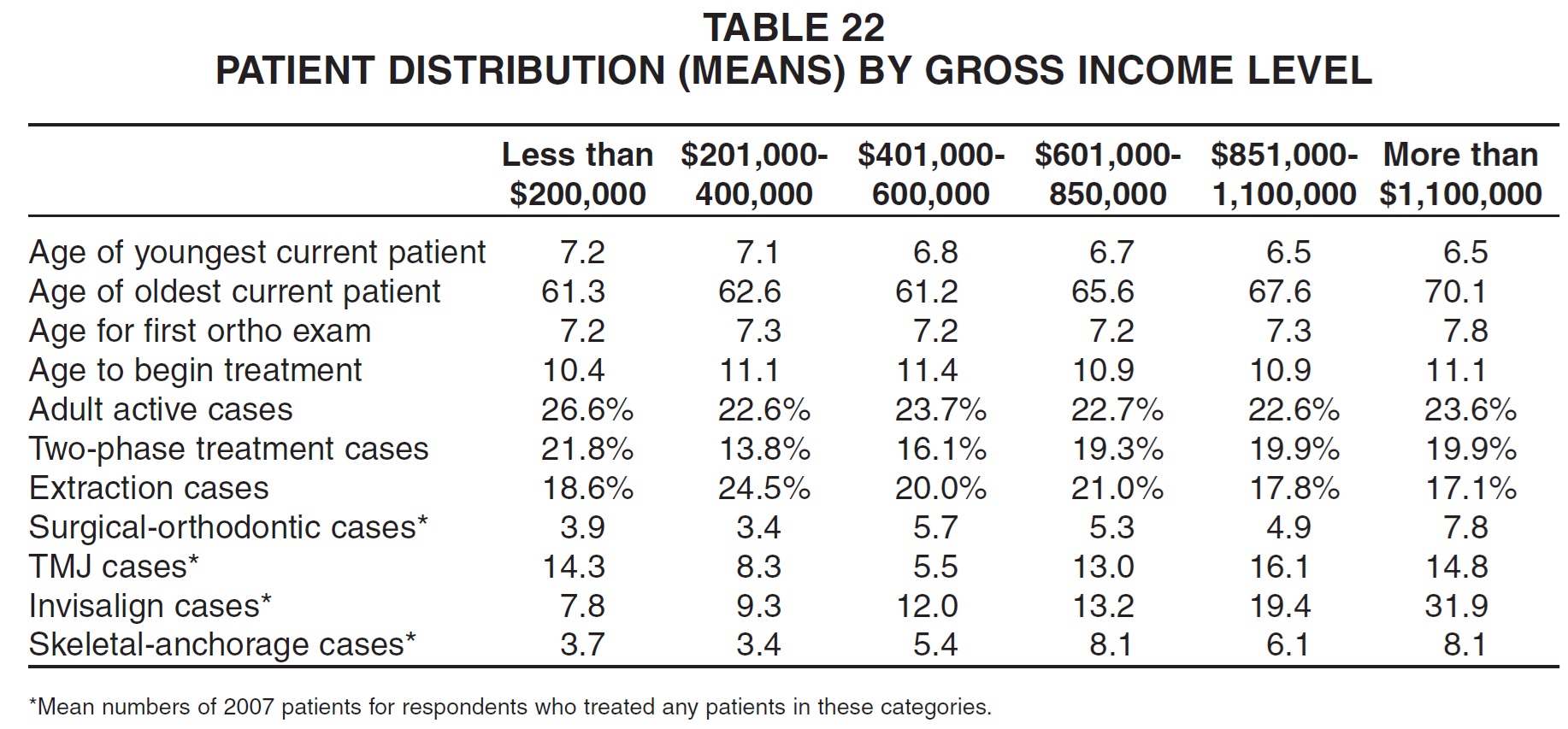
Practices with the highest gross income reported both the youngest and oldest patients and, as would be expected, the greatest mean numbers of patients in every category--with an especially wide gap in Invisalign patients (Table 22). They also treated the lowest percentage of extraction cases. The smallest practices in terms of gross income showed the highest percentages of two phase cases.
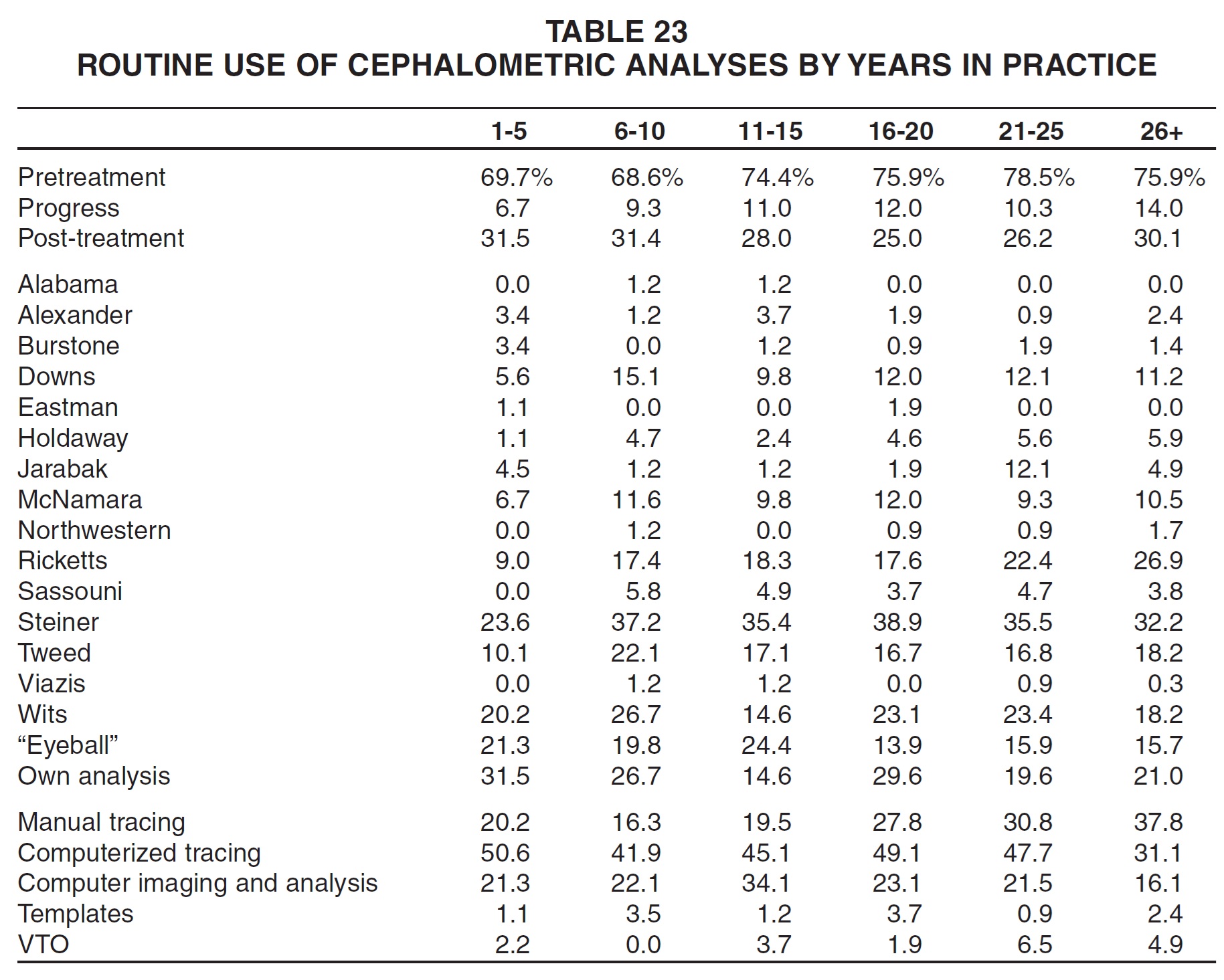
Diagnostic Records Older practices were more likely to use pretreatment and progress cephalometric analyses, but younger practices were slightly more likely to perform routine post-treatment analyses (Table 23). The oldest practices reported the least routine use of computerized tracings and imaging and the most routine use of manual tracings. The newest practices were less likely than others to use traditional analyses such as Downs, Ricketts, Steiner, and Tweed, and more likely to use their own analyses.
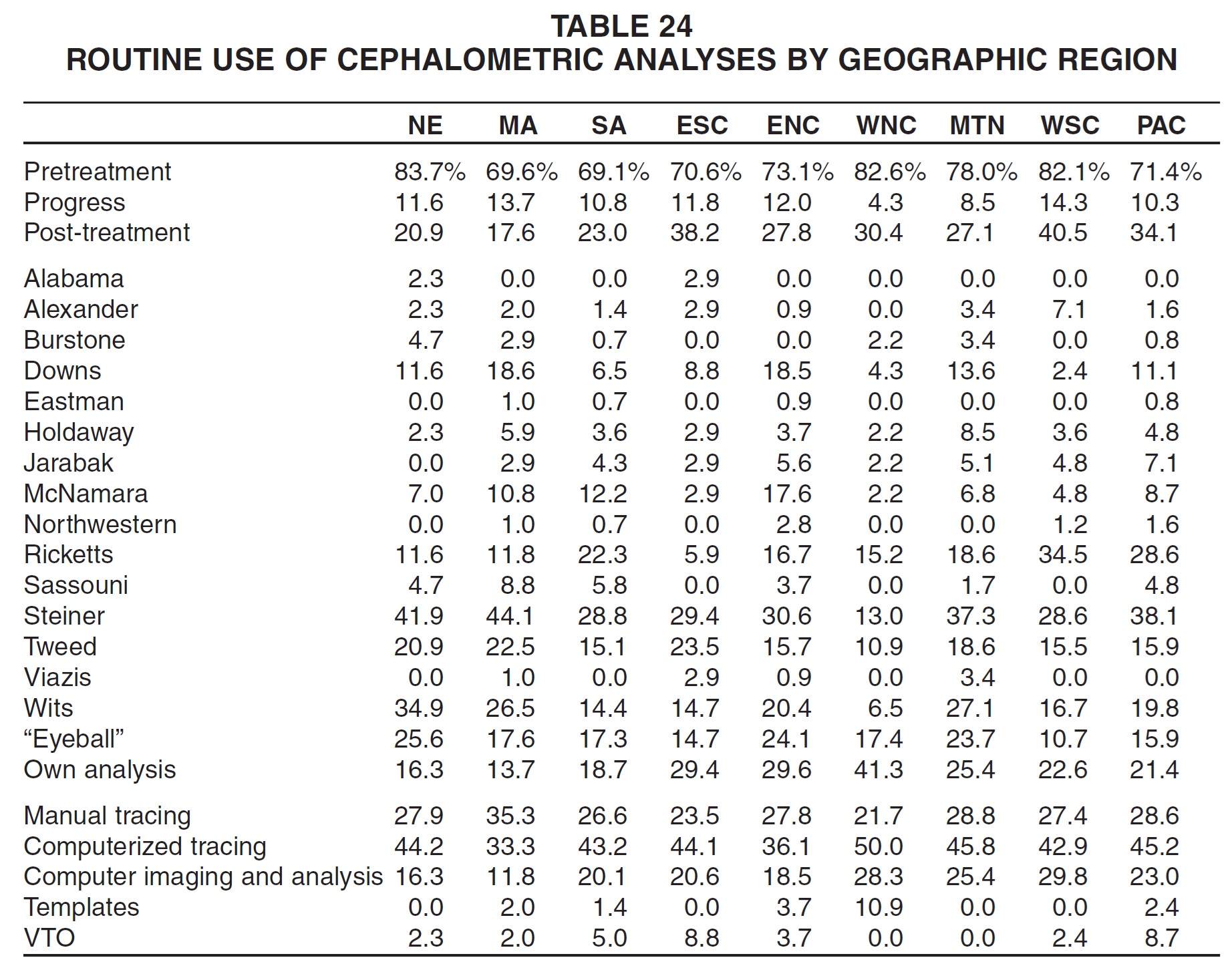
As in past surveys, there were obvious regional differences in the routine use of cephalometric analyses, at least partly based on the home of the originator (Table 24). The Alabama and Tweed analyses were used most routinely in the East South Central region; the Alexander and Ricketts analyses in the West South Central region; the Burstone and Wits analyses in New England; the Downs, Eastman, Sassouni, and Steiner analyses in the Middle Atlantic region; the Holdaway and Viazis analyses in the Mountain region; the Jarabak analysis in the Pacific region; and the McNamara and Northwestern analyses in the East North Central region.
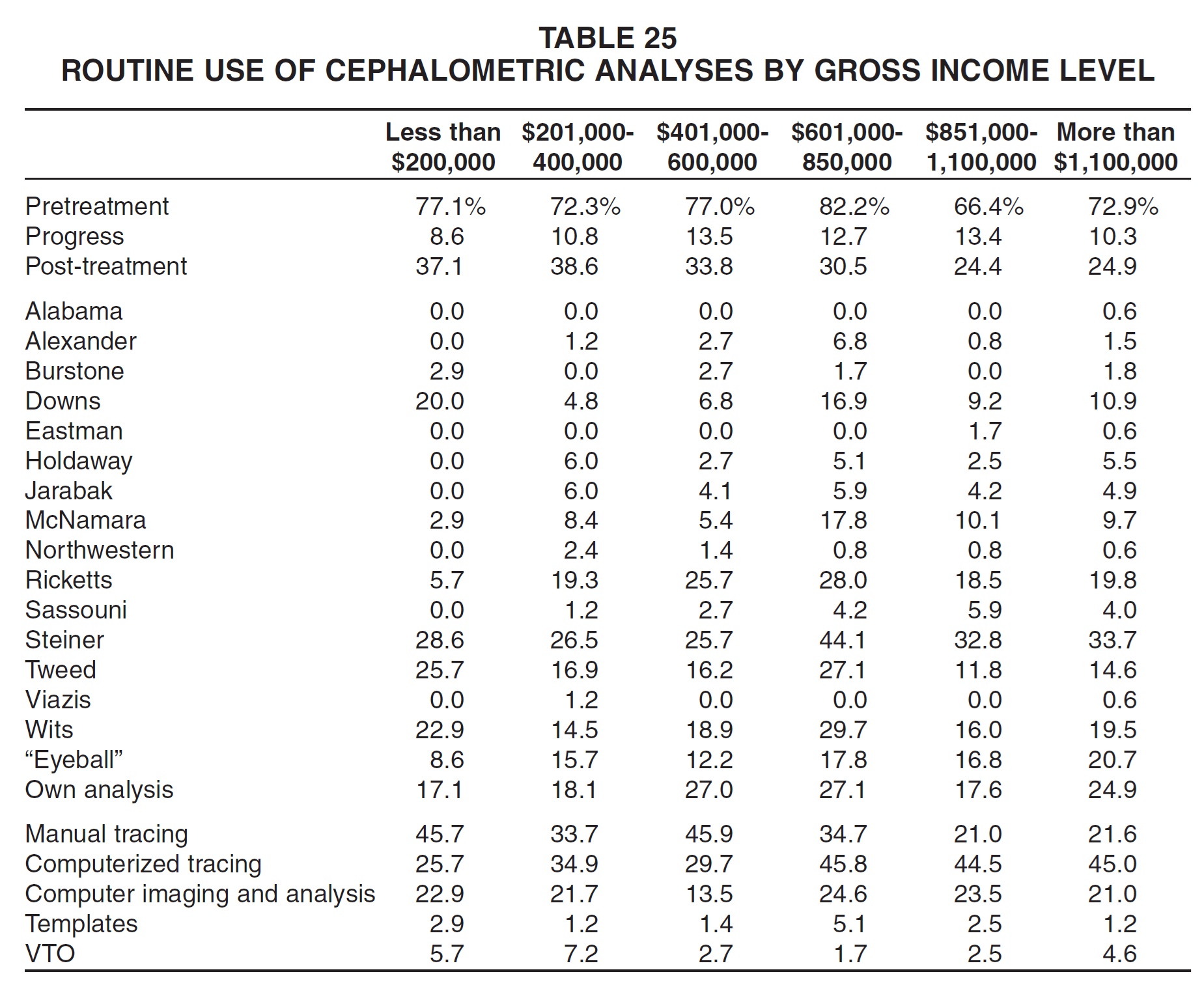
Respondents with higher gross income were generally more likely to use computerized tracings and less likely to use manual tracings and routine post-treatment tracings (Table 25). There were no noticeable patterns in the use of specific analyses according to income level.
Fixed Appliances
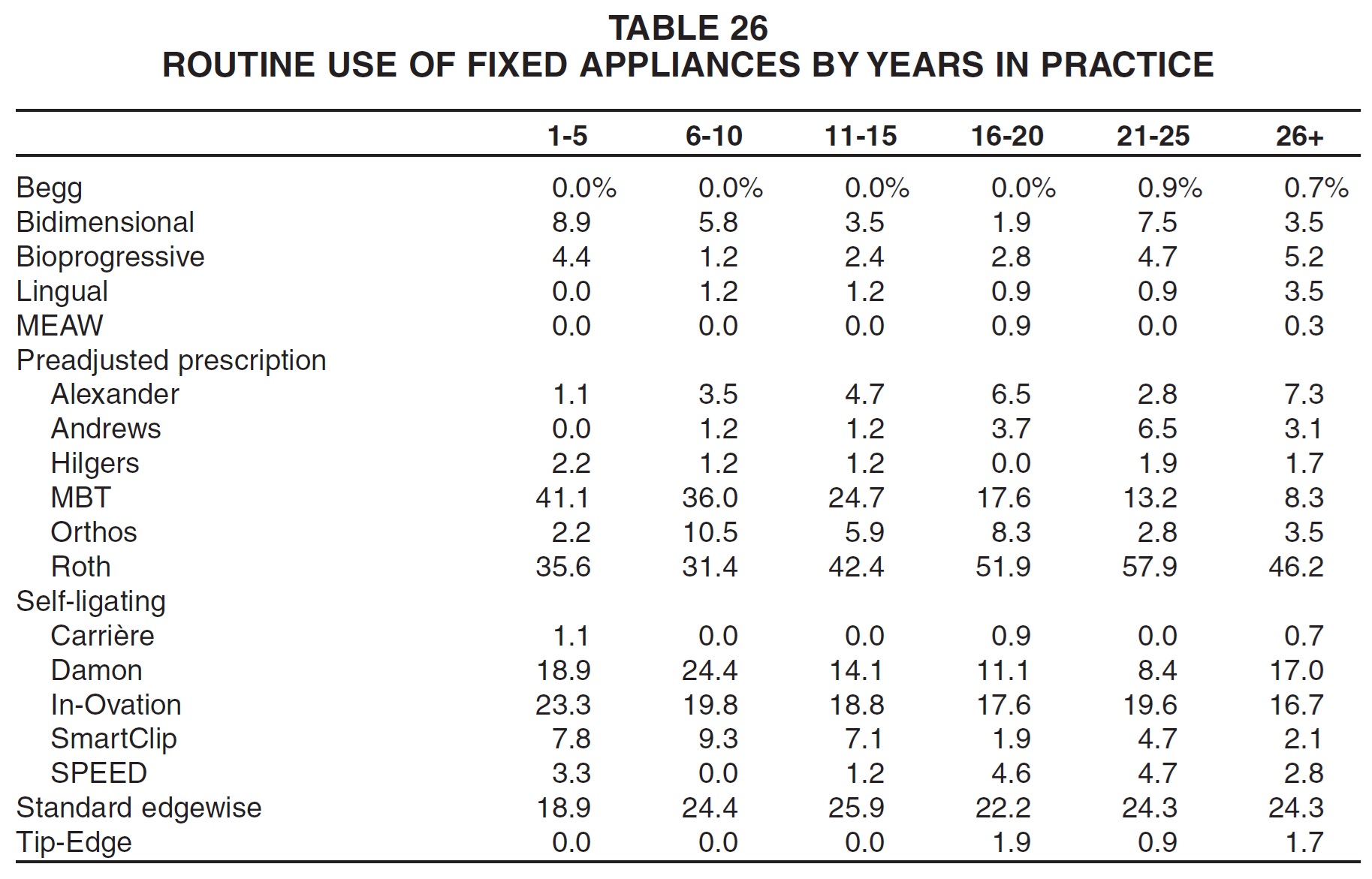
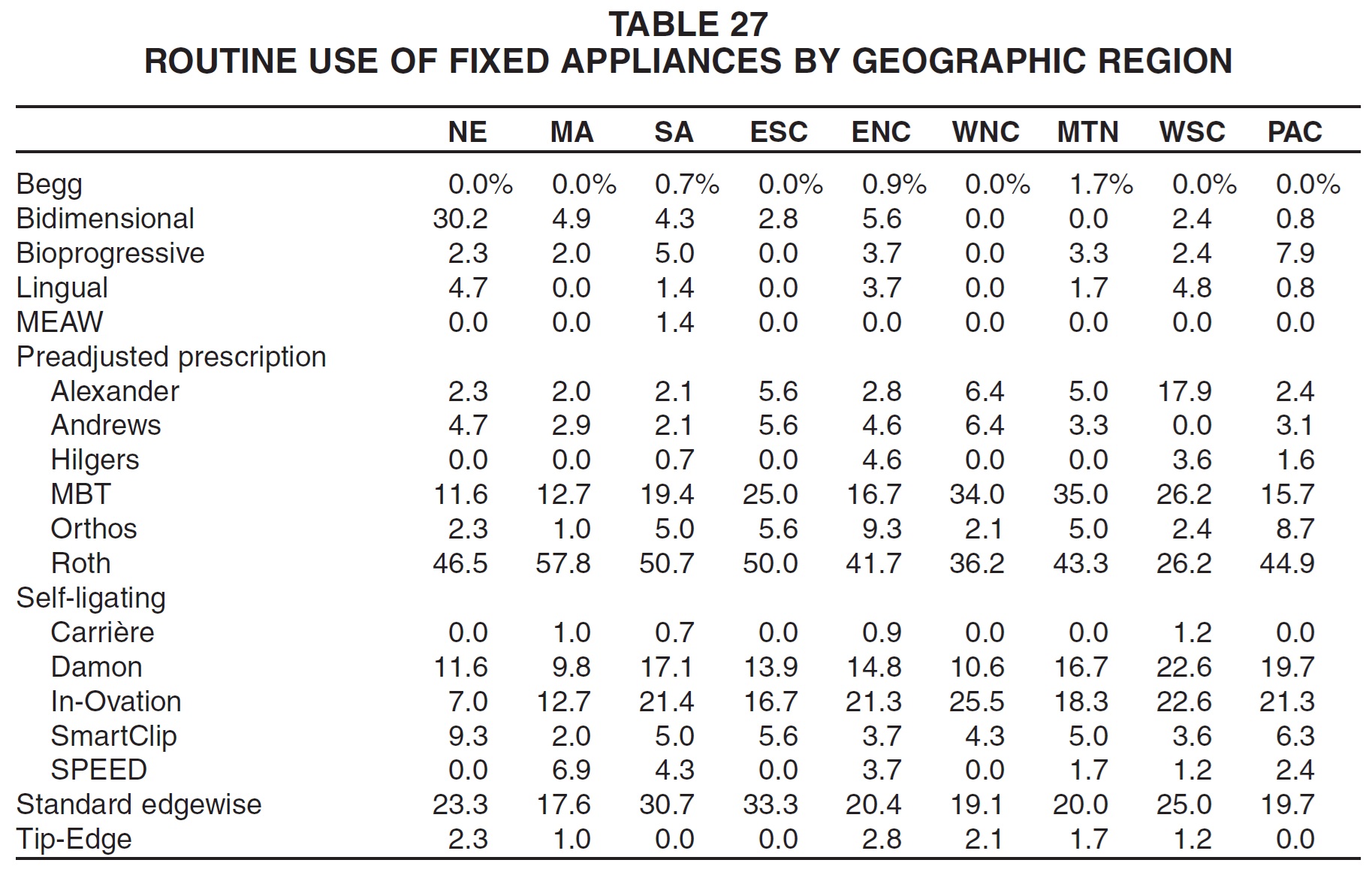
Regional differences could also be seen in the routine use of fixed appliances (Table 27). Bidimensional appliances were used by far the most commonly in New England. Of the other fixed appliances employed by at least 5% of the respondents in any region, the Bioprogressive system was used most routinely in the Pacific region; Alexander and Damon in the West South Central region; Andrews and In-Ovation in the West North Central region; MBT in the Mountain region; Orthos in the East North Central region; Roth and SPEED in the Middle Atlantic region; SmartClip in New England; and standard edgewise in the East South Central region.
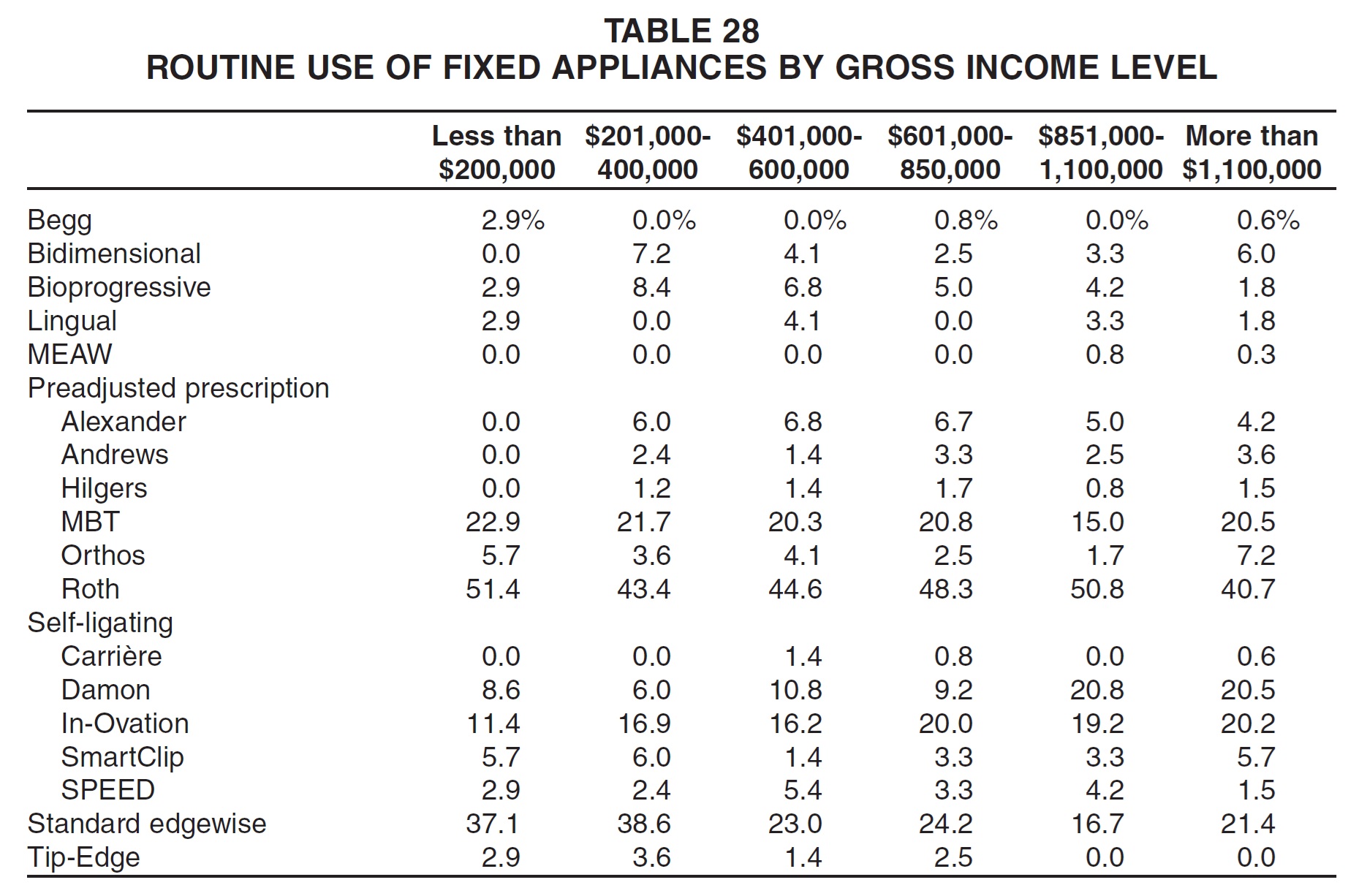
In general, the practices with lower gross income were more likely than practices with higher gross income to use standard edgewise appliances, and less likely to use self-ligating brackets (Table 28). Practices with the lowest gross income were also the most routine users of MBT and Roth prescriptions.
Brackets
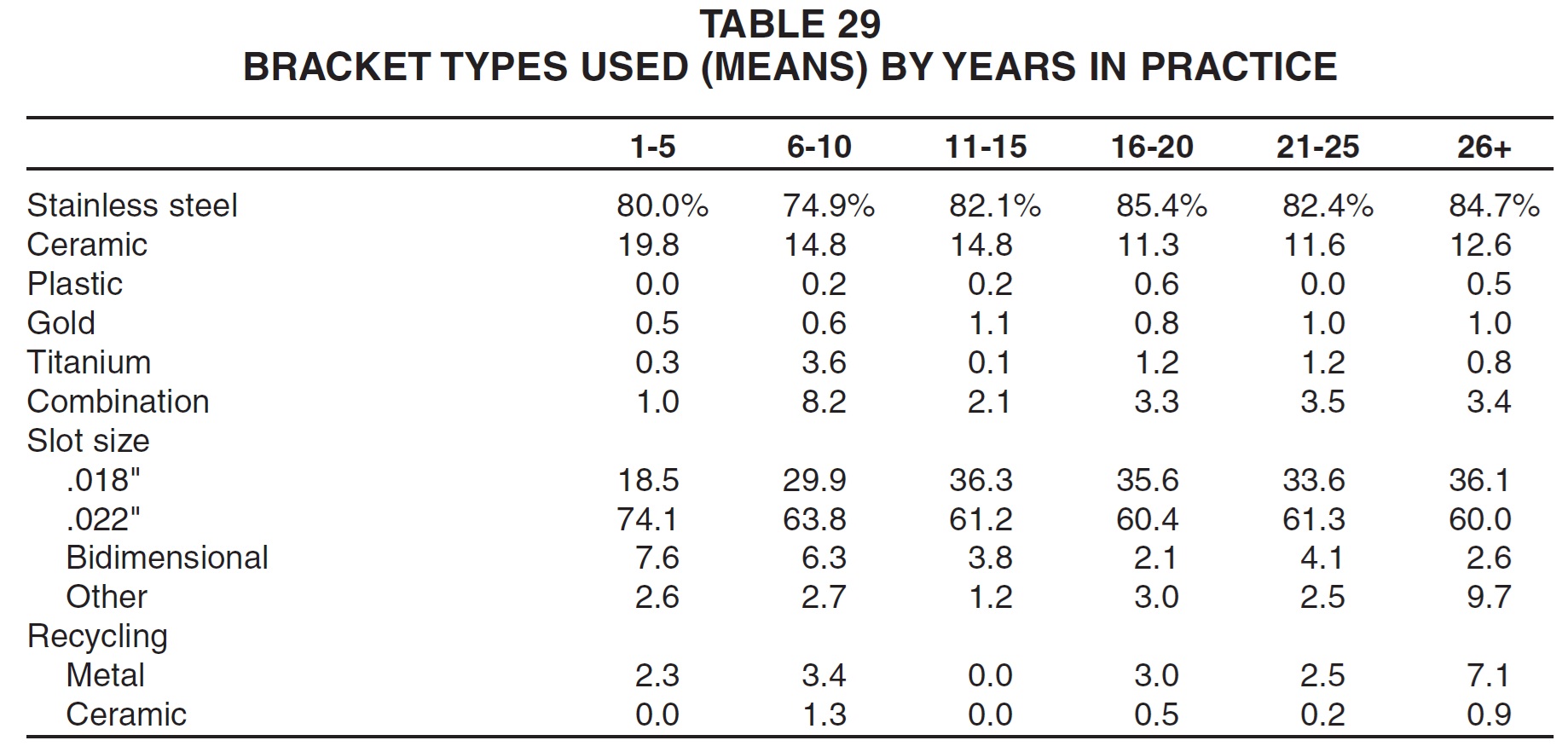
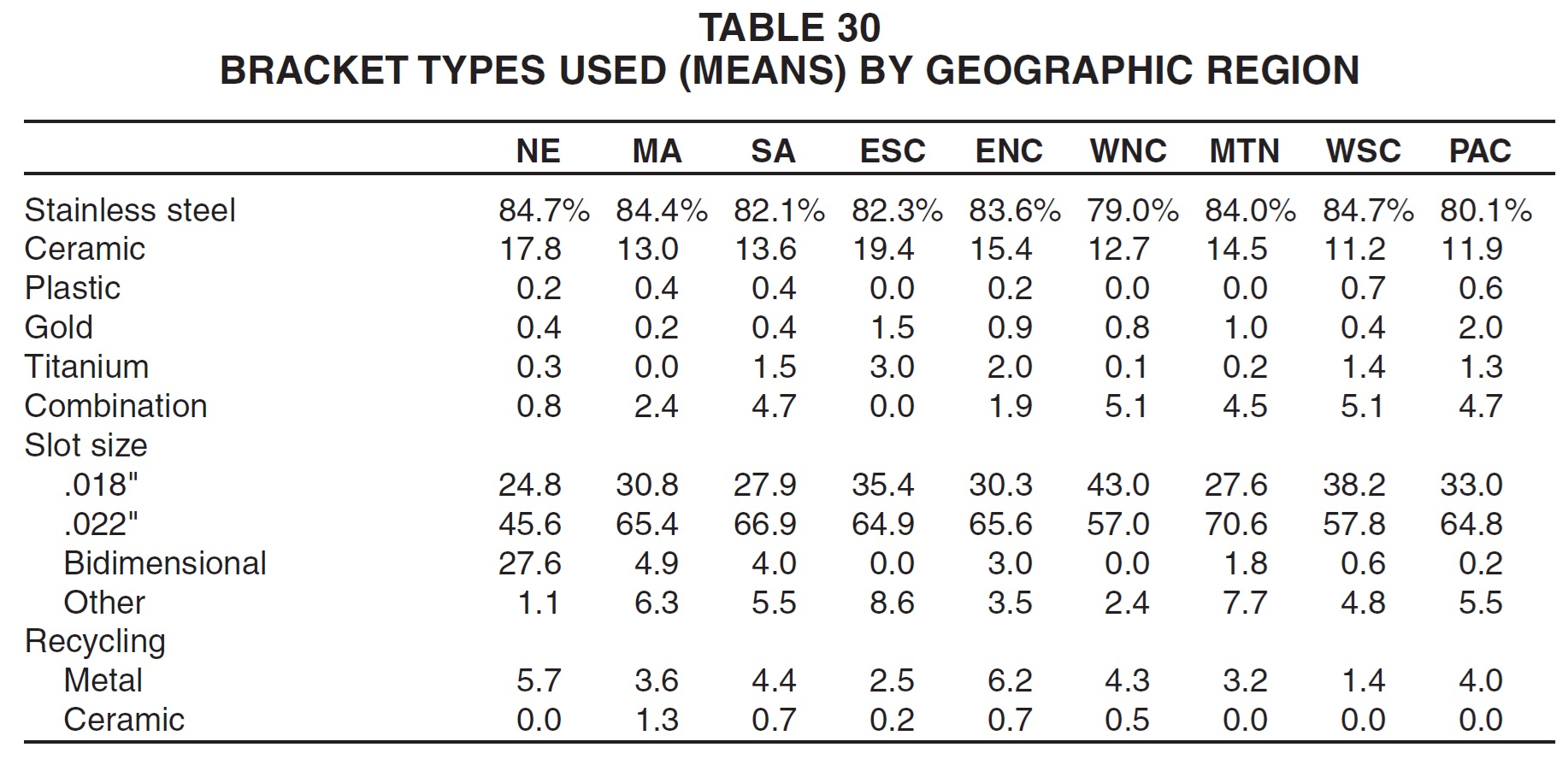
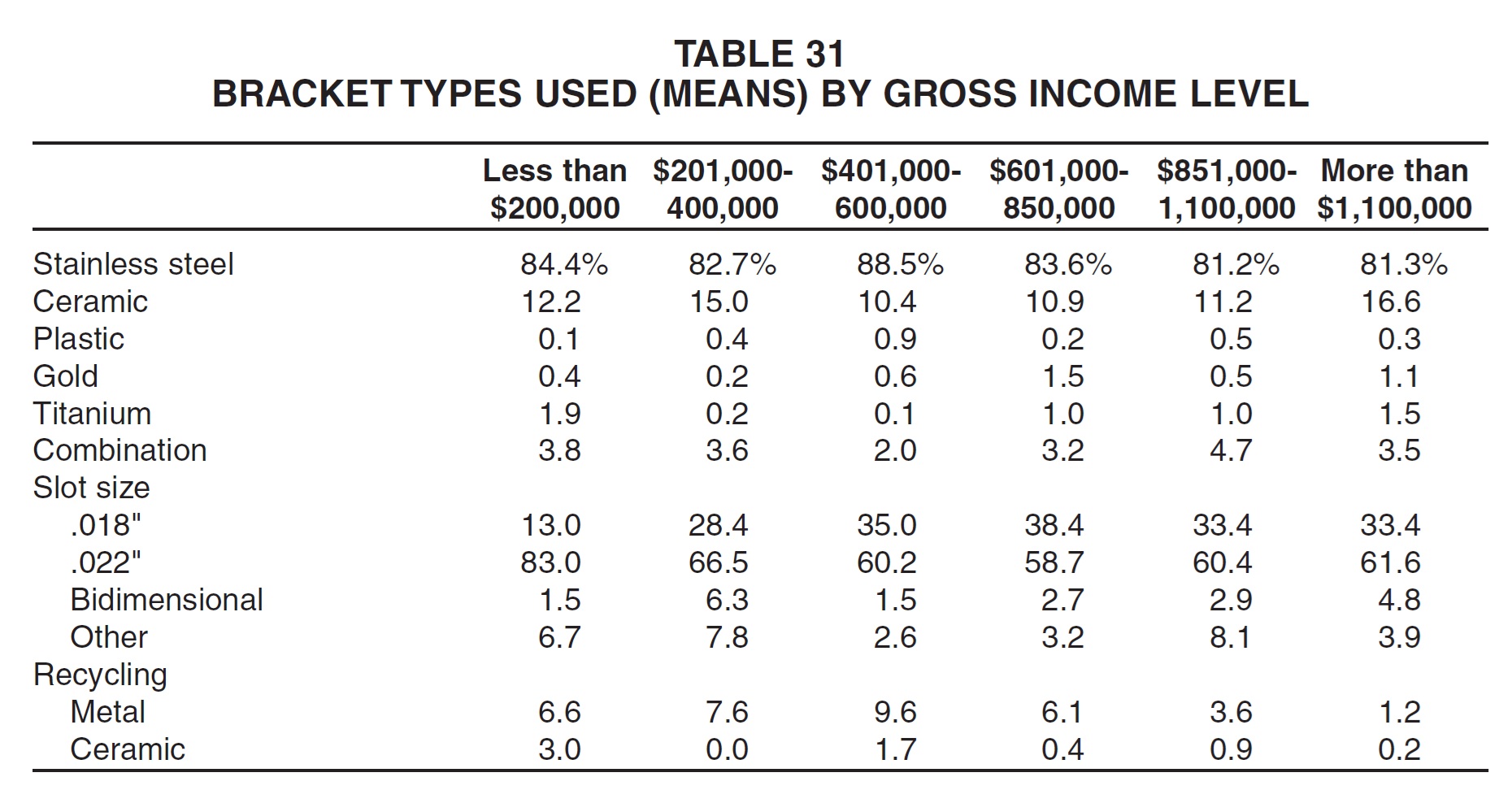
Respondents with the lowest gross income were by far the most likely to use .022" bracket slots (Table 31). Middle-income practices tended to use more stainless steel brackets and fewer ceramic brackets than their colleagues did, and they also reported recycling a higher percentage of their metal brackets.
Adhesives
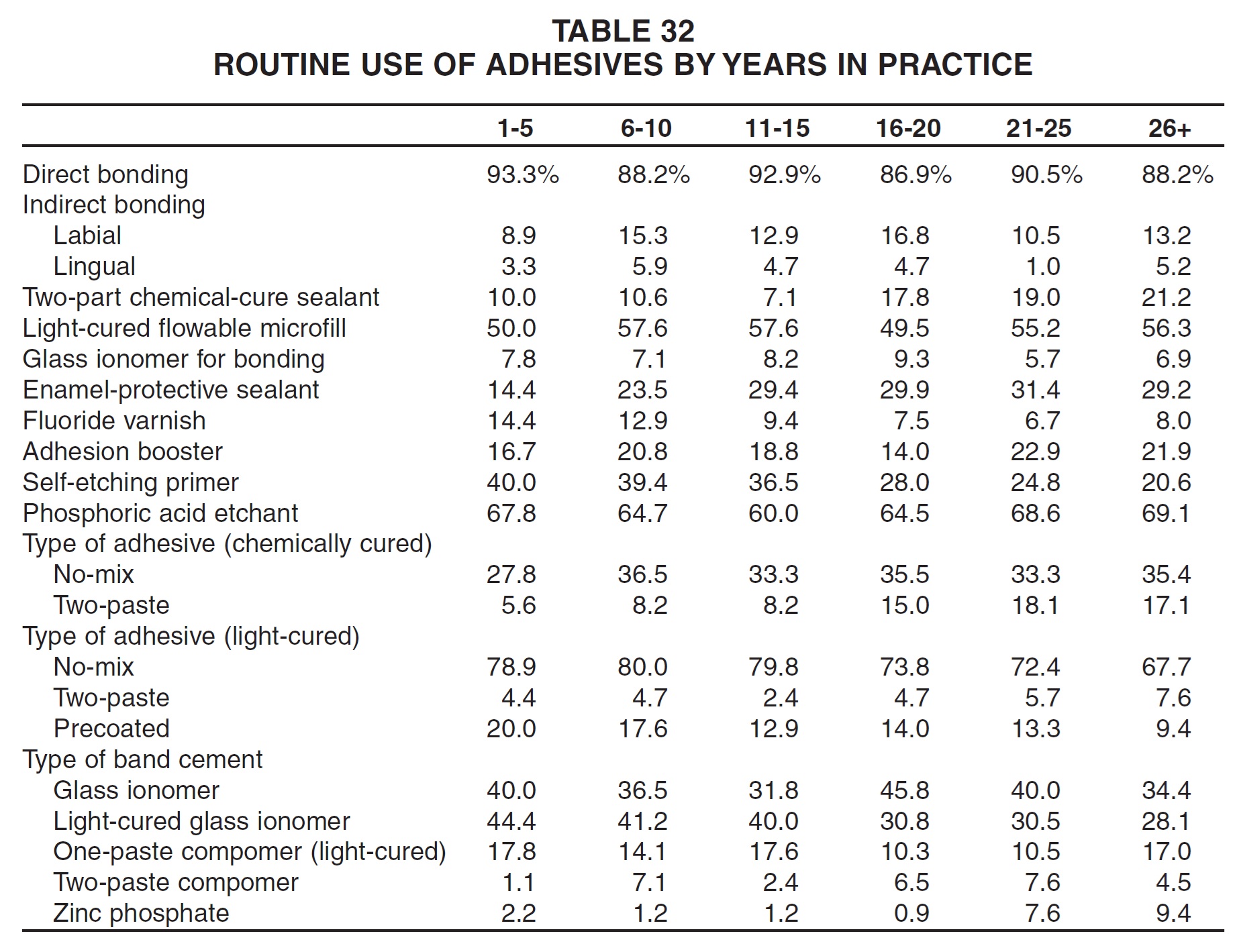
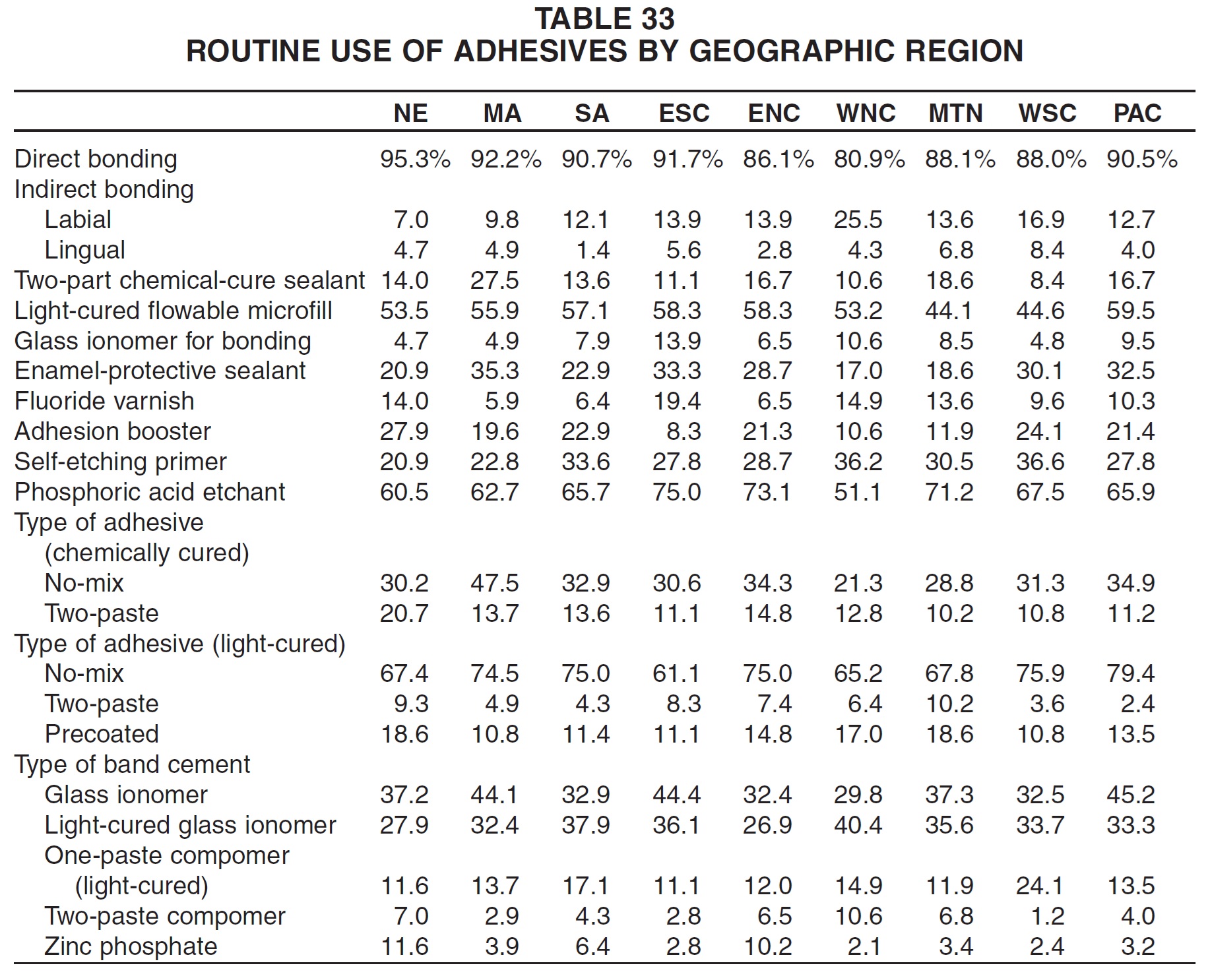
Direct bonding was used most frequently in New England; indirect bonding was most popular in the West North Central region (Table 33). Middle Atlantic respondents were most likely to use sealants and chemically cured adhesives.
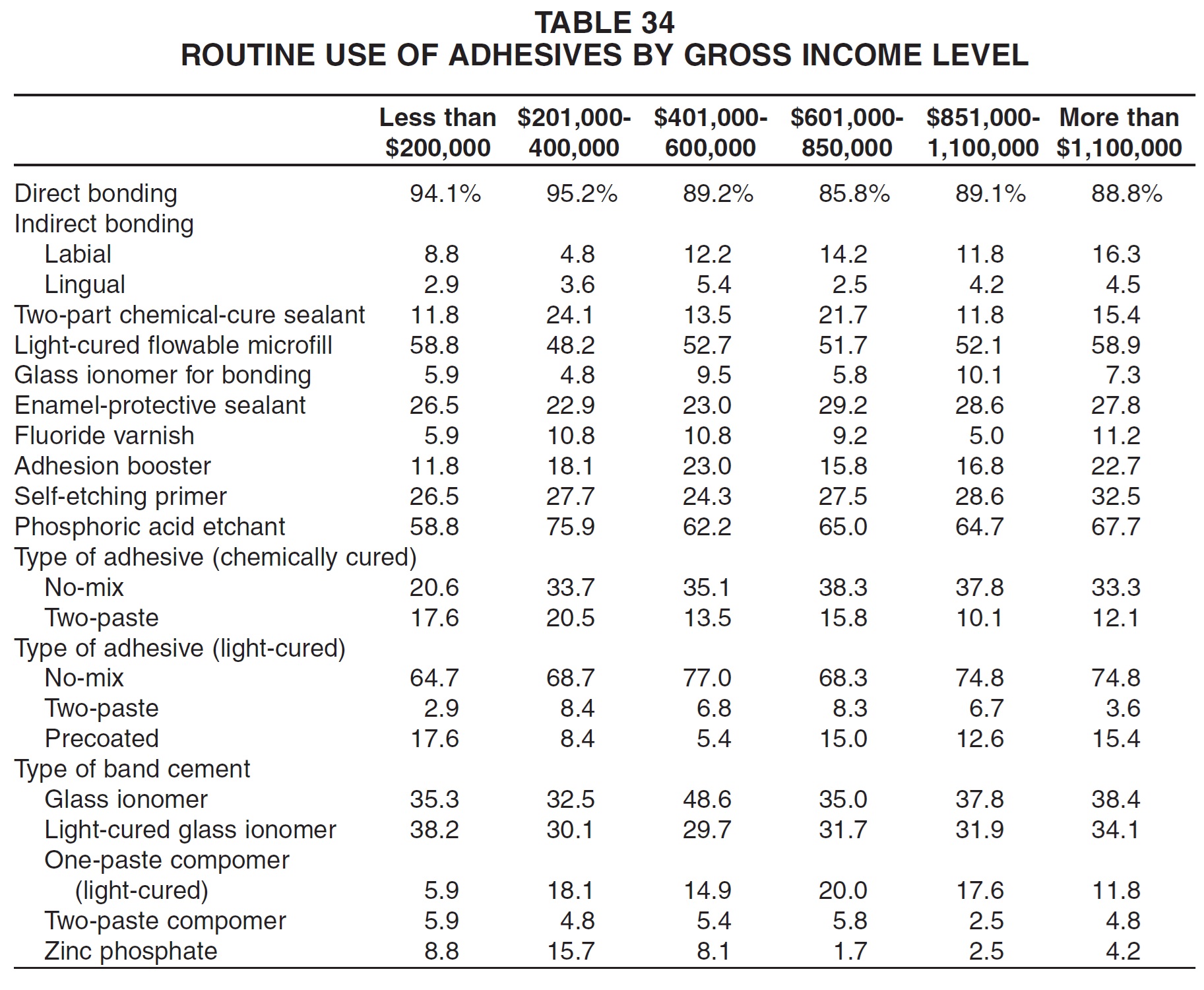
Higher-income practices were more likely than others to bond indirectly rather than directly (Table 34). Use of other adhesive methods did not appear related to gross income level.
Archwires
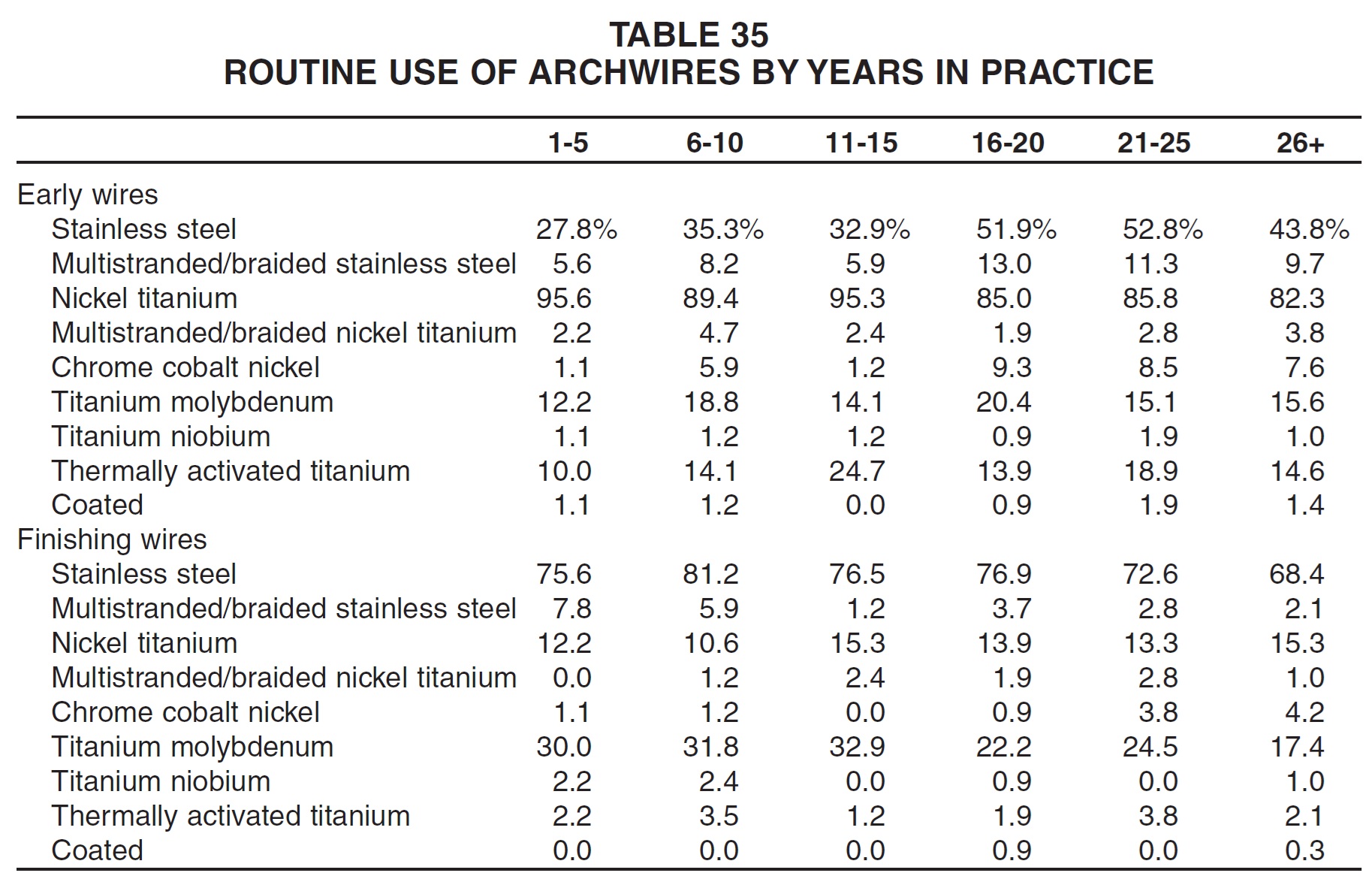
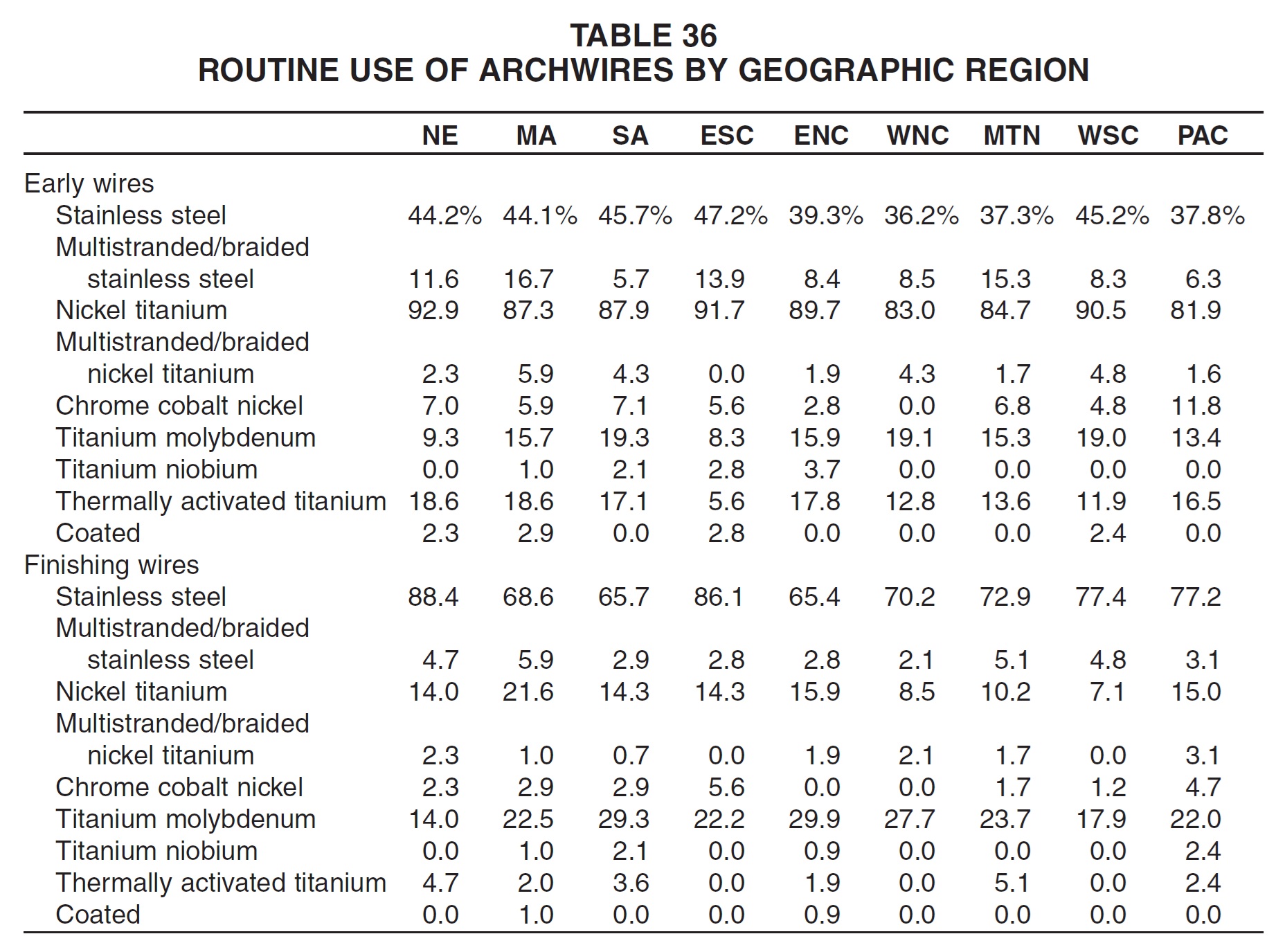
New England practices were the most routine users of nickel titanium initial archwires, but also of stainless steel finishing archwires (Table 36). East North Central practices were the least likely to use stainless steel finishing wires and the most likely to use TMA finishing wires. East South Central practices used stainless steel wires most routinely in the early stages, and were second to New England in the routine use of stainless steel finishing wires.
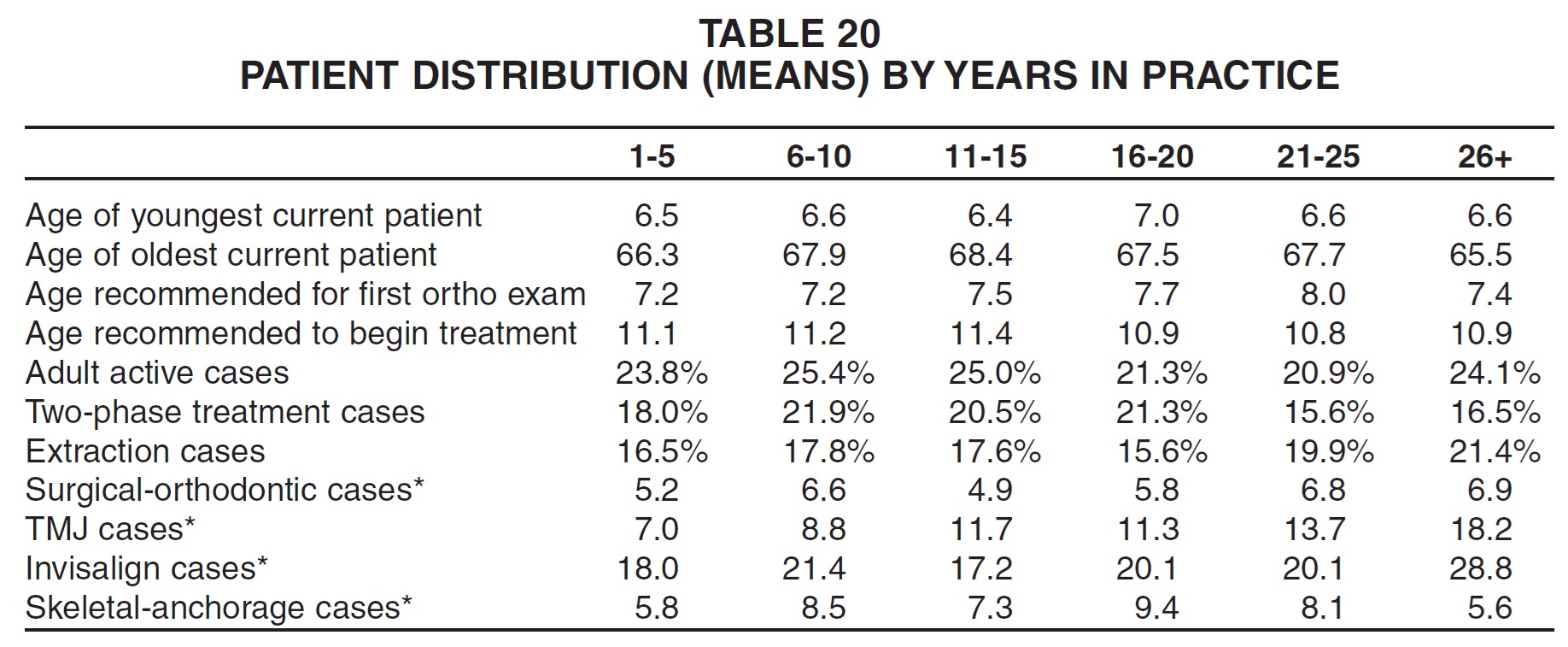
Respondents with the lowest gross income were the most likely to use stainless steel initial archwires and the least likely to use nickel titanium initial archwires (Table 37). On the other hand, they were the most likely to use nickel titanium finishing archwires (although only 20% of them used these wires routinely). Practices with higher gross income tended to use TMA wires more often for finishing.