The Readers’ Corner is a regular feature of JCO in which orthodontists share their experiences and opinions about treatment and practice management. Questions are sent periodically to JCO subscribers selected at random, and the responses are summarized here.
PETER M. SINCLAIR, DDS, MSD
What is the biggest challenge you have faced in dealing with the COVID-19 situation? Please explain how you dealt with the problem.
JCO readers identified four main challenges, with no particular concern predominating.
- Obtaining personal protective equipment (PPE), along with the problems of cost and becoming accustomed to wearing it.
- Fear of COVID-19 infection among both staff and patients, resulting in staff refusing to return and patients declining to come for appointments.
- Communication with patients about the new clinical and office guidelines.
- Scheduling patients back after the shutdown, with a reduced number of appointment slots to accommodate a significant backlog.
Fewer respondents offered specific suggestions for managing these problems, and there were no clear or common solutions.
Representative comments included:
- “Obtaining PPE: our suppliers ran short, so we started ordering wherever we could find it (Amazon) and paid huge mark-ups.”
- “Managing families’ expectations—be it rescheduling after a seven-week closure, altered projected treatment completion, or new procedural plans (closed waiting room, checking in from the car, limited siblings allowed, etc.).”
- “Once we reopened, we were working at a reduced capacity and had to extend hours and days to make up for the backlog of patients. It will take a few more months to catch up on the fixed-appliance cases.”
Similar articles from the archive:
What is your best piece of advice for other clinicians at this time?
The two predominant themes were to diligently follow all safety protocols and to keep things simple in both clinical treatment and patient explanations.
Specific remarks included:
- “Always follow PPE rules and wear protection appropriately, while scheduling your appointments so that you have time to disinfect fully between each patient.”
- “For PPE supplies at a good cost, check out the N95 project for practitioners; also Mari’s List. Cross-train all staff at all times. You need less staff if you are seeing fewer patients.”
- “Understand that safety must be a priority and that all the work must be organized in a different way than before the pandemic.”
- “Our patients and families appreciate the precautions we are taking (CDC, ADA, AAO), prescreening, temperatures, etc. Stay calm. We can and are able to work during this pandemic.”
- “Keep treatment simple. I think you can use a lot of different appliances to get the job done. Keep it simple for you and your patients.”
- “Continue to stay informed and speak confidently to your team and your patients. They are being showered with fearmongering through social media and their friends. Continue to discuss what the science is showing, and remind them to stay vigilant in all aspects of their lives.”
- “Let our smile change the world; let us not let the world change our smile.”
What extra patient and family precautions are you taking?
Most practices reported using most, if not all, of the following precautions:
- Parents waiting in the car and texting before patients come in.
- COVID-19 medical history and consent forms (from AAO) prior to entry.
- Temperature screening and hand sanitizers at the door.
- Limited non-patient access (for example, one parent only, no siblings).
- Mask requirements for all patients and accompanying persons.
- Closed waiting rooms, or only limited and well-spaced seating.
- Closed restrooms and toothbrushing areas.
- Plexiglass barriers at the front desk to protect the staff.
- Masks for all staff, plus face shields for all clinical staff.
- Team scrubs and jackets laundered daily.
- Longer intervals between patients (50-75% of capacity).
- Requirement for every patient to rinse with hydrogen peroxide at the beginning of the appointment.
- Limiting aerosol procedures wherever possible.
- Use of high-volume evacuation (HVE) and a four-handed approach for all aerosol procedures.
- More remote monitoring of aligner patients.
Additional suggestions included the following:
- Using an air-purifying machine with ozone.
- Screening all patients with a pulse oximeter.
- Setting up enclosed operatories for aerosol-generating procedures.
- Placing plastic screens between chairs.
- Using automated appointment scheduling to avoid front-desk paperwork.
How did you communicate with your patients and referring doctors as to the enhanced precautions you are taking to protect your patients?
Most offices reported using two or three communication methods. Texting or e-mail was the most common, used by 83% of the practitioners; notices on the door were employed by 46%. Social media posts (40%) and website alerts (30%) were also quite popular, followed by voice calls when scheduling appointments (23%). Letters to referring doctors (13%) and online videos (10%) were less frequently used.
One particularly interesting comment:
- We provided a weekly set of newsletters, sent by text and e-mail and through online social media, describing all the logistical, equipment, and structural changes throughout the lockdown and then announcing our reopening on June 1. When we communicated that event, we also provided copies of articles, webinars, and interviews that the doctor had been involved with in the interim.
What new equipment did you buy in response to the COVID-19 situation?
Four items were commonly mentioned: ultraviolet disinfection systems, high-efficiency particulate air (HEPA) filters, disinfecting mist foggers, and HVE equipment. Some offices reported purchasing electric handpieces and additional autoclaves, and a few said they equipped private isolation rooms.
What special precautions have you taken in regard to aerosol-generating procedures?
Most of the respondents said they tried to limit aerosol-generating procedures as much as possible, either by assigning a specific space (at one end of the main clinical area or in a separate room, if available) or by allocating certain times on the schedule (often the last patient of the day). Also commonly mentioned was the use of HVE with special attachments, combined with a four-handed debonding protocol and N95 masks and face shields. A few clinicians reported using local ultraviolet or fogging measures.
Additional comments included:
- “In a separate room, at the end of the day, along with high-volume suction and N95 masks. We use a separate acrylic capsule that almost completely isolates the patient.”
- “Aerosol-generating procedures, such as removal of appliances and adhesives, are relegated to two private rooms with air-isolation filtration systems fitted with dual HVE attachments and electric handpieces operating at low RPM without water.”
What percentage of your staff did you lay off or furlough during the COVID-19 shutdown? What percentage did you rehire upon reopening?
Fully 65% of the practices reported that they either laid off or furloughed most of their staff during the COVID-19 shutdown. Many offices retained one or two staff members to answer phones and handle administrative tasks. Of the practices that laid off employees, 77% said they rehired the entire staff upon reopening; the rest retained 65-90% of the original staff.
Specific comments included:
- “Nine of 12 employees were furloughed. We kept two (one per office) to handle phones and emergencies, and one treatment coordinator for virtual exams and observations.”
- “All the staff were on unemployment for two weeks. When we got our Paycheck Protection Program (PPP) loan, they went back to their normal salary. 100% stayed with us.”
- “I did not lay off any employees; however, three out of 10 sheltered themselves. I rehired two of the three and added three more employees.”
- “I laid off 100% and put two on very limited hours (four hours per week) to help with phones and emergencies. I tried to rehire them all, but one refused to come back.”
Have you had any staff decline to return to the office because of COVID-19 fears? What has been your response?
Two-thirds of the practitioners reported that none of their staff declined to return. For the remaining 33%, it was usually only one employee who declined to return. Retirement was the most common reason given, followed by age (over 55), ongoing systemic conditions, pregnancy, and childcare limitations. The doctors’ responses were generally sympathetic, wishing the employees well and giving them the opportunity to return when they were ready and comfortable.
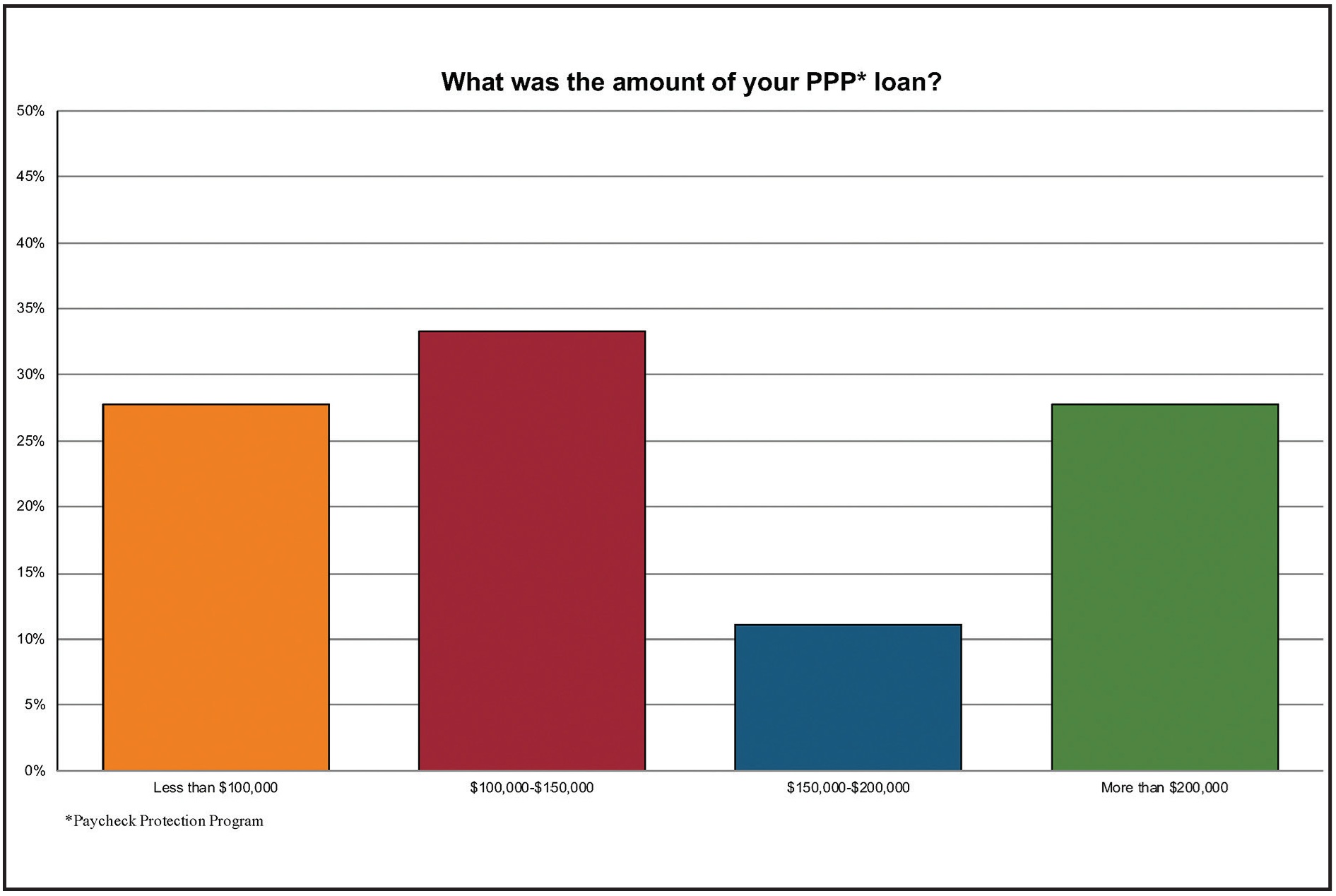
Did you obtain a PPP loan? If so, what was the amount?
Of the U.S. respondents, 85% reported receiving a PPP loan. The most common amount was between $100,000 and $150,000, but answers varied considerably.
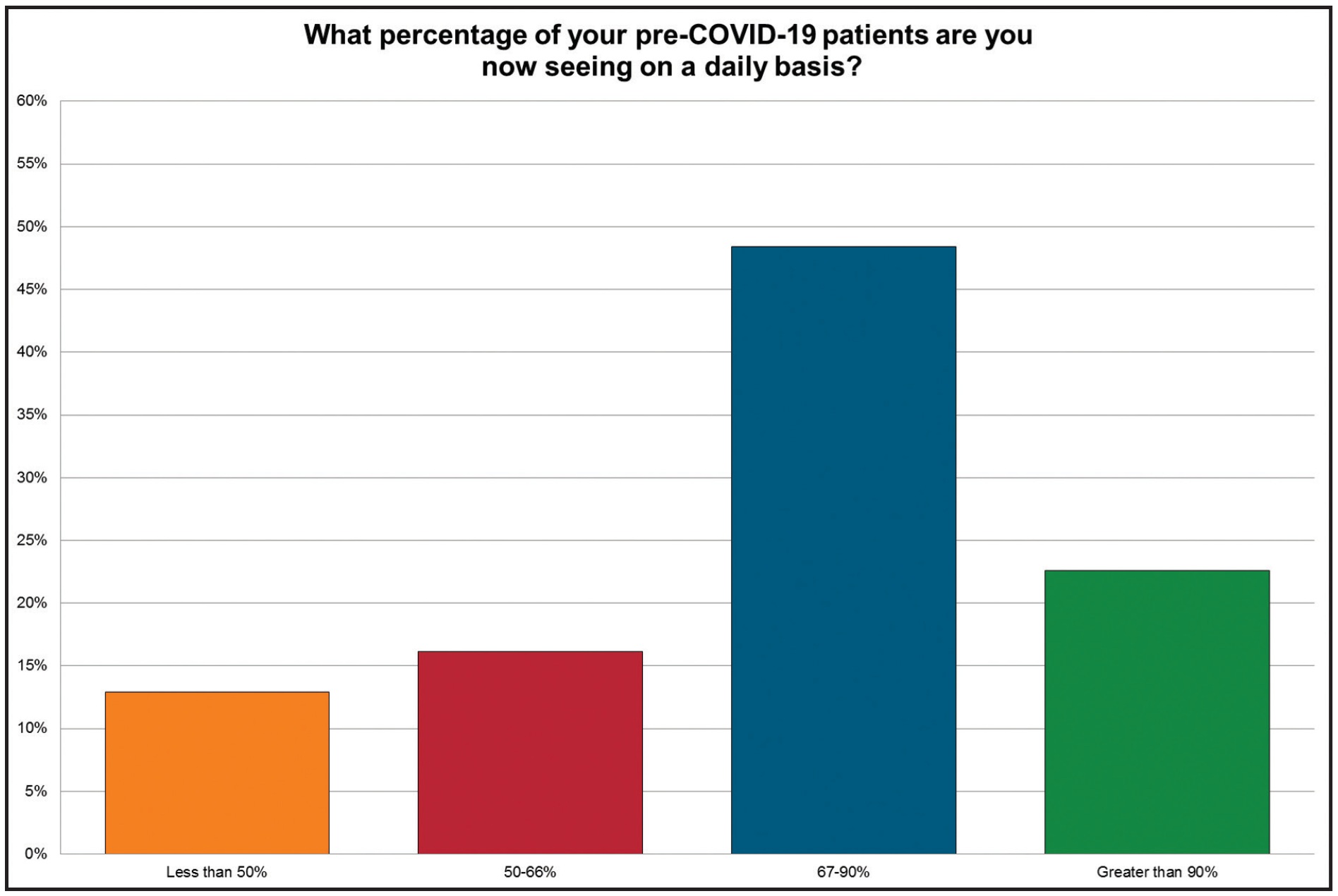
What percentage of your pre-COVID-19 patients are you now seeing on a daily basis?
A substantial majority of the practices said they were seeing at least two-thirds of their patients regularly.
What percentage of your patients have declined to return for treatment because of COVID-19 fears?
A little more than 80% of the offices reported that less than 10% of their patients had declined to return for treatment. About 16% noted 10-30% of their patients declining to return, while only one respondent had experienced a rate greater than 50%.
Compared to the same time period in 2019, how much of a drop have you seen in new patient starts?
Just under half of the practices reported small declines in starts (less than 10%); 29% reported declines in the 10-30% range, but nearly 20% reported major declines in new starts, ranging from 30% to 50%.
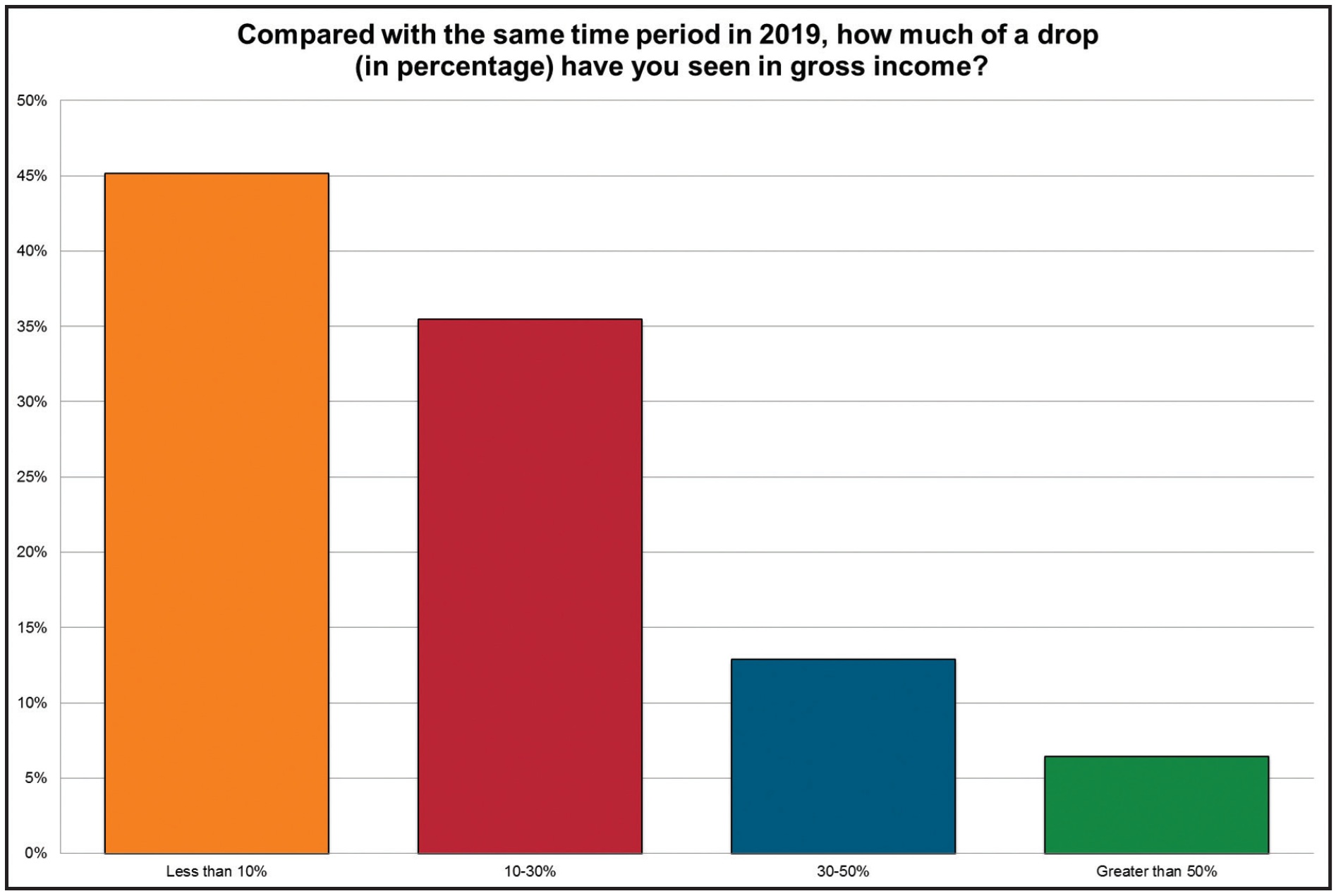
Compared to the same time period in 2019, how much of a drop have you seen in gross income?
Again, a wide range of responses was received, with 45% of the offices reporting a decline of less than 10% in income and 35% showing a 10-30% decline. On the other hand, almost 20% of the practices reported serious declines in gross income—more than 30% compared to last year.
Do you have any other comments you would like to share regarding your response to COVID-19?
Comments included:
- “I think there are many protocols that will remain with us forever. We must rethink the way we see patients and make them see that they really are our chief concern.”
- “Educate everyone around you. Give them confidence in tackling this situation.”
- “It revolutionized the whole world, and we should learn our lessons.”
JCO would like to thank the following contributors to this column:
Dr. Hessa Abdulla, Doha, Qatar
Dr. Noble Anderson, Lebanon, PA
Dr. Jay Bowman, Portage, MI
Dr. Wes Cardall, Bakersfield, CA
Dr. Carole Charavet, Liège, Belgium
Dr. Joe Dietrich, Canton, OH
Dr. Irma Dumbrytė, Vilnius, Lithuania
Dr. Fred Fenderson, Prescott, AZ
Dr. Allison Hamada, Metairie, LA
Dr. William Harrell, Alexander City, AL
Dr. James Hart, Cleburne, TX
Dr. Douglas Harte, Livingston, NJ
Dr. Haval Jalal, Erbil, Iraq
Dr. Jean Kay, Maumee, OH
Dr. Neal Kravitz, South Riding, VA
Dr. Rohit Kulshrestha, Mumbai, India
Dr. Laura Lineberry, Boise, ID
Dr. Mark Lowe, Fresno, CA
Dr. Elizabeth Lyons, Seattle, WA
Dr. Andrew Marshall, Greer, SC
Dr. Melissa Milligan, Burlington, Ontario
Dr. Alexandros Moullas, Thessaloniki, Greece
Dr. Sadia Naureen, Islamabad, Pakistan
Dr. Natalie Parisi, Wyomissing, PA
Dr. Sharmila Shetty, Mangalore, India
Dr. William Valdes, Santiago, Chile
Dr. Michael Willes, Carlsbad, CA



