ALIGNER CORNER
Evaluating the Efficacy of Lower Incisor Intrusion with Clear Aligners
This new JCO column is compiled by Contributing Editors Robert L. Boyd, DDS, MEd, and William V. Gierie, DDS, MS. Every few months, they will address an area of clear-aligner therapy of interest to our readers. Your suggestions for future topics or authors are welcome.
In this first installment of the Aligner Corner, the authors evaluate the efficacy of lower incisor intrusion using the Invisalign* system. They obtained pre- and post-intrusion lateral cephalometric records from 30 consecutive adult patients treated by two experienced Invisalign practitioners. All cases involved SmartTrack* material and two-week aligner change intervals. No bite ramps were used in any of the patients.
The authors acknowledge that the small sample size, lack of randomization, and retrospective design were problems, but they provide thorough data on their intraobserver reliability and measurement error. Their results show that the average amount of incisor intrusion obtained with aligners was 73% of the amount requested. From this, they devised a formula to aid in predicting the amount of intrusion that should be prescribed in the ClinCheck.* I found the data intriguing and wonder if a sample treated with bite ramps would show more reliable intrusion.
WVG
Similar articles from the archive:
Evaluating the Efficacy of Lower Incisor Intrusion with Clear Aligners
Patients are increasingly requesting esthetic and comfortable alternatives to conventional orthodontic treatment with brackets and archwires.1 To meet this demand, orthodontic manufacturers have introduced (or reintroduced) clear plastic brackets, tooth-colored ceramic brackets and archwires, lingual brackets, and clear aligners. Esthetic improvements in orthodontic appliances are often associated with reduced efficiency, however, due to the new materials involved and the need to revise treatment mechanics. To produce an optimal outcome, the orthodontist must recognize, accept, and compensate for these changes.
Despite the real or imagined limitations of clear-aligner therapy, it is the most requested esthetic treatment option in many practices. As a removable appliance, an aligner is useful in patients challenged by bracket breakage and oral-hygiene issues.2,3 Aligner therapy has also been shown to require significantly fewer visits, a shorter treatment duration, fewer emergency visits, and less emergency and total chairtime compared to conventional edgewise braces.4
Early aligner therapy was restricted to passive retention or correction of minor crowding and rotations. Improvements in diagnosis and treatment planning, mechanics, and materials were needed to treat such routine orthodontic problems as impacted teeth, severe crowding requiring extractions, and accompanying occlusal discrepancies. Patient demand for clear aligners (primarily Invisalign) resulted in an unprecedented involvement of clinicians in the development of new techniques, such as attachments designed for specific individual tooth movements. Meanwhile, the manufacturer significantly improved its software, clinical support, and aligner materials.
Incisor Intrusion with Clear Aligners
Proponents of clear aligners believe technological advances have now enabled predictable correction of deep overbites.5 Depending on individual case requirements, this necessitates intruding the incisors to a level functional occlusal plane (absolute intrusion), extruding the buccal segments with little or no intrusion of the incisors (relative intrusion), or a combination of both. In Burstone’s view, absolute incisor intrusion is the treatment of choice for patients with vertical growth tendencies.6 Whether this can be reliably achieved with clear aligners is still a subject of controversy.
An integral aspect of Invisalign therapy is its virtual treatment-planning software, ClinCheck, which demonstrates the specific tooth movements required to idealize each patient’s occlusion and allows the clinician to sequence these movements to maximize efficiency. Although the software builds in .25mm of intrusion per tray, experienced Invisalign providers are acutely aware that virtual ClinCheck treatment does not always accurately represent clinical results. To compensate, they usually add a significant amount of overcorrection to their virtual treatment plans. The definitive amounts of overcorrection needed for various tooth movements have not yet been determined.
Measuring the actual anterior intrusion obtained with Invisalign as a percentage of the amount requested in ClinCheck, Nguyen and Cheng reported a mean accuracy of 79%.7 In contrast, Kravitz and colleagues found a mean accuracy of only 46.6% for lower central incisor intrusion, causing them to state that “correction of deep overbite with Invisalign appears unlikely”.8 Rossini and colleagues, in a systematic review of studies relating to orthodontic tooth movement with clear aligners, determined that they could be used to treat simple malocclusions with “light overbite discrepancies”.9 These authors concluded that clear aligners can produce anterior intrusive movement comparable to that achieved with a preadjusted fixed appliance.
The studies cited above were all completed prior to the release of Invisalign’s SmartTrack aligner material, which was designed to provide better control and tracking, more constant force, higher elasticity, more precise aligner fit, and improved patient comfort.10 This material—combined with precision bite ramps, optimized bite attachments, and new pressure areas—may offer a greater potential for opening deep bites. The purpose of the present study was to evaluate the efficacy of lower incisor intrusion with SmartTrack aligners compared to the amount of virtual tooth movement requested in ClinCheck. Another goal was to develop a formula for incisor intrusion that could be programmed into ClinCheck treatment plans.
Materials and Methods
Orthodontic treatment records of 30 consecutively treated non-growing adult patients were analyzed in this longitudinal retrospective study. Twenty records were from a private practice in Nashville, Tennessee, and 10 from a private practice in Minneapolis. Each practitioner had more than 10 years of experience treating patients with Invisalign.
In an effort to reduce sample variability, cases were selected using the following criteria:
- Non-growing, non-syndromic adult.
- No previous orthodontic treatment.
- Normal to deep-bite malocclusion.
- Nonsurgical treatment plan.
- Diagnostic-quality pre- and post-treatment lateral cephalograms.
- SmartTrack aligner material only.
- Aligners changed at two-week intervals using the standard .25mm of intrusion per tray.
- No use of bite ramps or other auxiliary treatment modalities.
Consecutively treated patients meeting these criteria comprised 11 males and 19 females, with a mean starting age of 29.4 (range of 18-63).
Landmarks for all cephalometric measurements were located by one investigator and verified by one of the co-investigators. The vertical position of the lower incisors was measured in relation to the bony structure of the mandible from lateral cephalometric films taken at T1 (initial) and T2 (post-treatment). First, the most anterior lower incisor (crown tip and root apex) was identified on the pretreatment cephalogram. To standardize measurements, the incisor was traced along this axis using a Steiner Lateral Cephalometric Tracing Template.** The lower border of the mandible was then traced from the vertical midpoint of the posterior border of the ramus to B point, including the internal border of the symphysis. Finally, the mandibular plane was traced as a line tangent to the lower border of the mandible. The position of the lower incisor at T2 was identified in the same manner as at T1. The pretreatment tracing was superimposed over the post-treatment cephalometric tracing, oriented on the mandibular border and registered on the internal symphysis landmarks (Fig. 1).
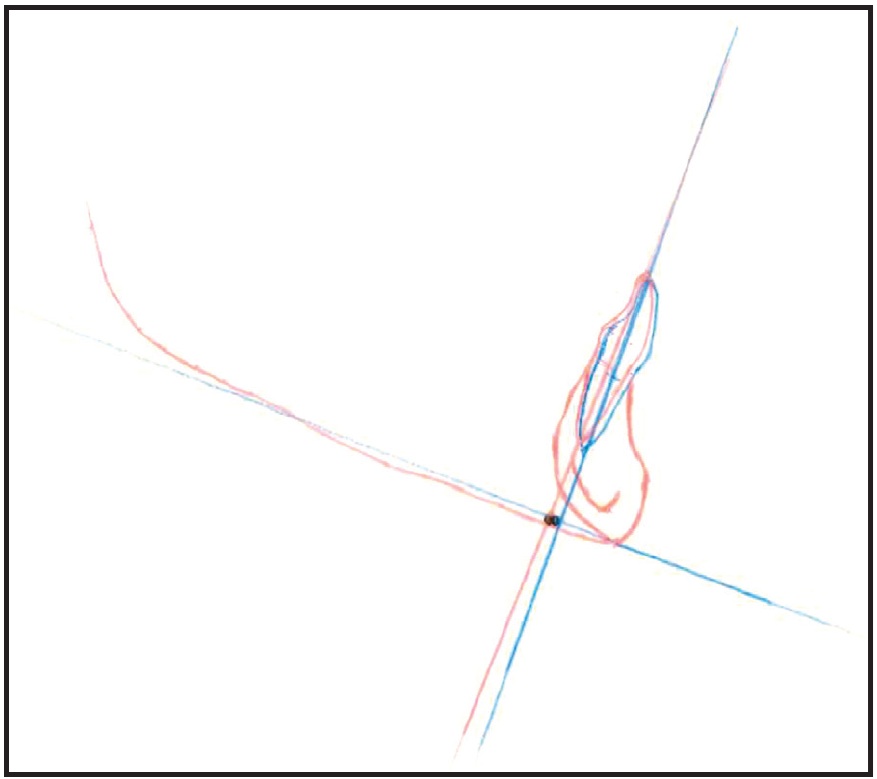
Fig. 1 Sample lateral cephalometric superimposition used to measure amount of intrusion obtained with clear aligners.
The center of resistance (CR) of the traced lower incisor was identified as the point halfway between the crest of the alveolar bone and the root apex.11 The CR was transferred from the pretreatment to the post-treatment cephalogram. The distance from CR to the mandibular plane was measured with digital calipers, accurate to .01mm, on a line along the long axis of the tooth. The distances at T1 and T2 were then compared to determine the amount of intrusion of the lower incisor at CR.
To test intraobserver reliability, the lateral cephalograms were retraced and remeasured four weeks after the first tracing. The repeated measurements were statistically compared using the method recommended by Bland and Altman12 and the intraobserver agreement index proposed by Filippi and colleagues13:
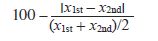
The mean intraobserver reliability was found to be 99.98% (95% confidence interval, 99.94, 100) with a mean arithmetic difference between measurements by the same observer of .001mm (95% confidence interval, −.055, .057).
The total amount of intrusion requested for the most anterior lower incisor in ClinCheck, including any refinements, was obtained directly from Invisalign. Statistical analysis was used to compare the amount of actual intrusion obtained to the amount requested in ClinCheck. The null hypothesis for this study was that the amount of incisor intrusion requested in ClinCheck is equal to the amount of incisor intrusion obtained clinically.
Results
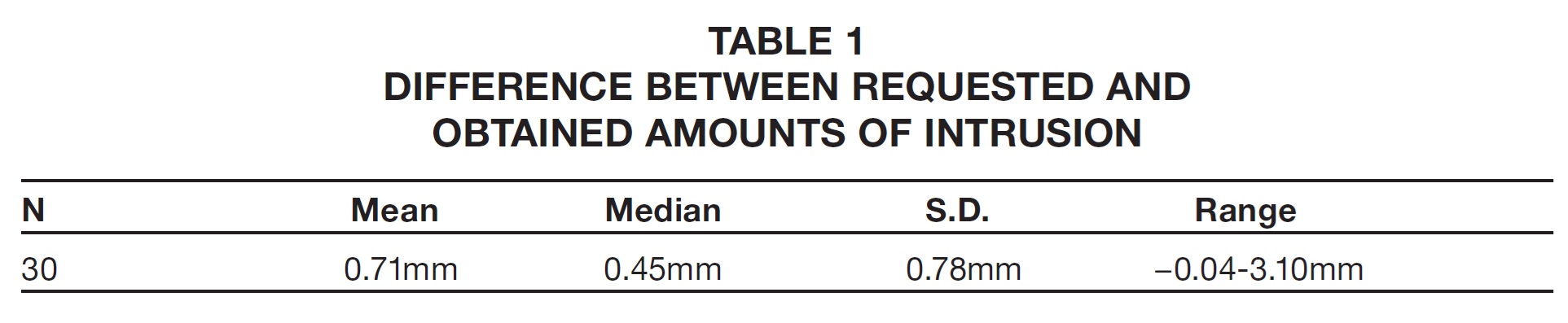
For each patient, the observed intrusion was recorded and the difference between the requested and observed values was calculated (Table 1).

A simple histogram demonstrated that the differences were not distributed normally, but appeared to be skewed to the right (Fig. 2).
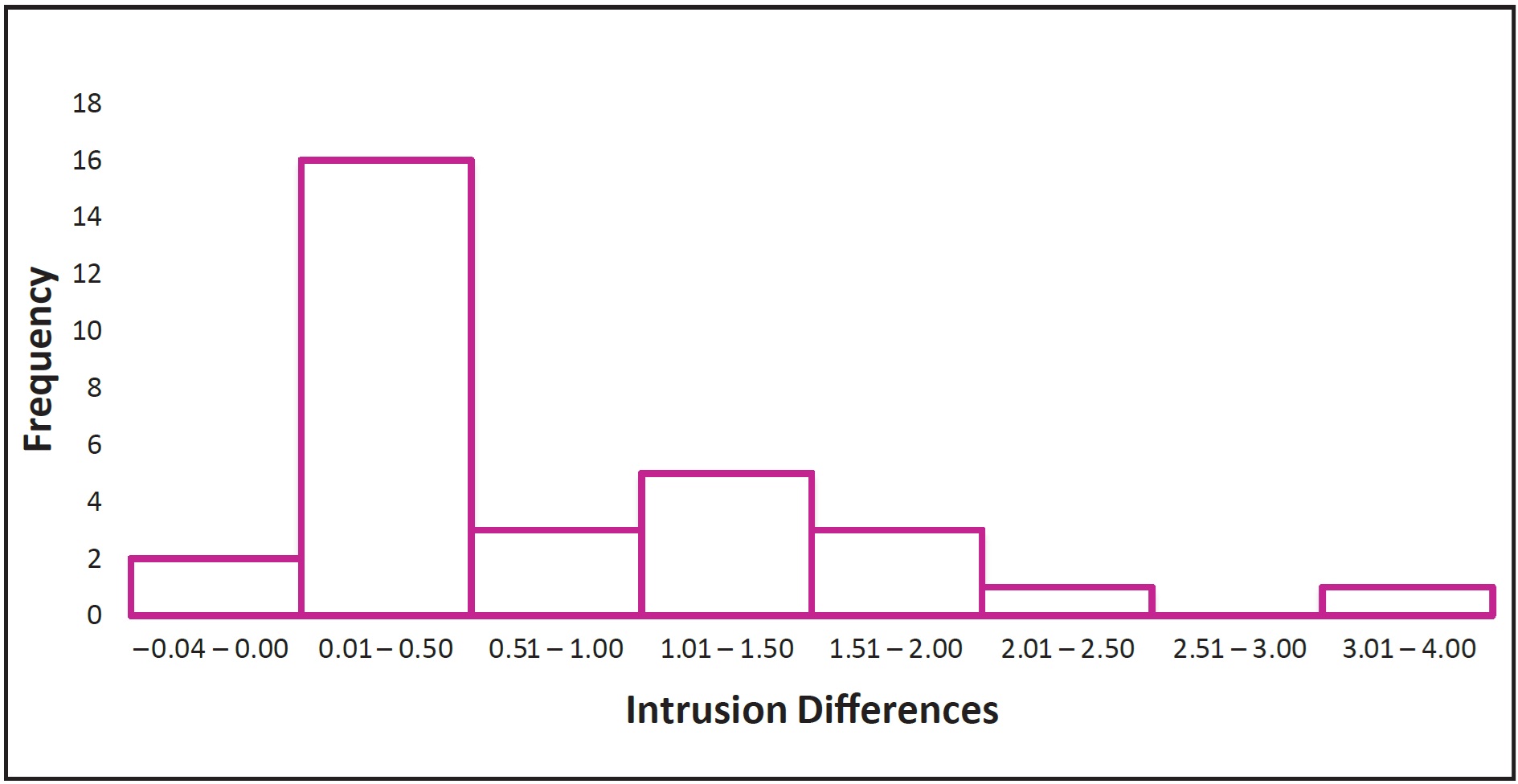
Fig. 2 Histogram of differences between requested and obtained amounts of intrusion (mm).
Because the sample size was nearly the minimum required to invoke the Central Limit Theorem, and because hypothesis tests of the mean based on Student’s t-test distribution are considered unacceptable by many, a hypothesis test of the mean was conducted to assess the extent of the differences. Even though there were nine differences of less than .1mm, ranging from −.04mm to .06mm, the remaining 21 differences ranged from .18mm to 3.10mm.
A t-test of the mean was then conducted with an alternative hypothesis: that there is a difference between the amount of intrusion requested vs. what is obtained (Table 2).
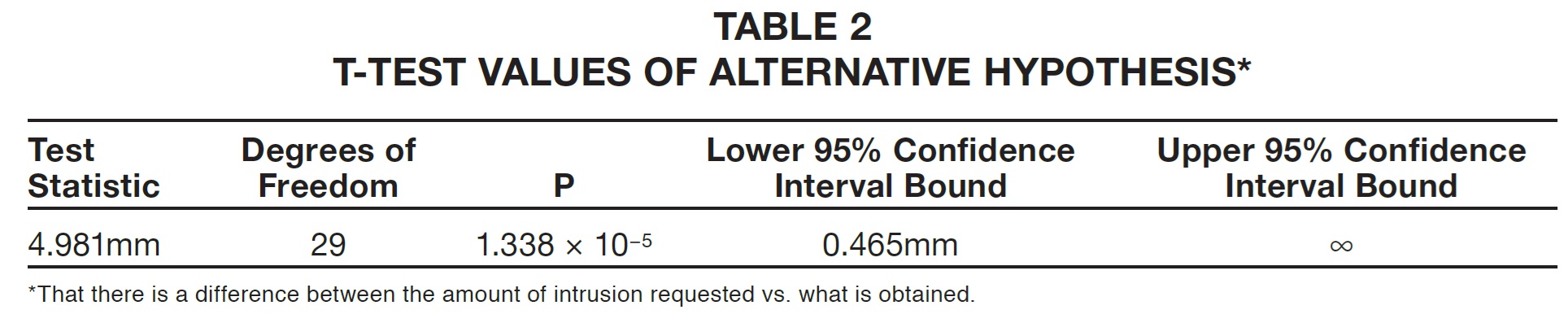
Based on this test, we could reject the null hypothesis that there is no difference between the amount of intrusion requested vs. what is obtained. The mean difference was clearly greater than 0mm. In fact, according to the confidence interval, we could be 95% confident that the indicated interval, starting at .465mm, contained the true mean difference.
Using a least-squares linear model, we can predict the observed intrusion (ŷ) for a given requested intrusion (x). We can also create a confidence interval for the predicted value (taking into account the variation in the data), in the form used for a 95% confidence interval14:
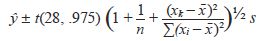
where xk is a specified requested intrusion and s is the square root of the sum of the squared residuals. Note that the further the requested intrusion gets from the mean, the larger the confidence interval becomes, making predictions more precise in the middle of the requested intrusion data significant and less so toward the upper and lower bounds of the data.
Assuming a valid regression model, we can use the inverse function of the regression equation to estimate the required overcorrection in incisor intrusion, solving for the independent variable in the original linear model to obtain:
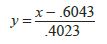
where x now represents the actual correction needed and y represents the requested correction (including overcorrection). This simplified equation can therefore be used as a rough estimate for the amount of intrusion that should be requested in ClinCheck.
Discussion
The mean amount of incisor intrusion requested in ClinCheck was 2.19mm, but the mean amount of intrusion obtained clinically was 1.49mm, resulting in a mean difference of .71mm and a mean intrusion accuracy of 73%. This is similar to the 79% general intrusion accuracy reported by Nguyen and Cheng,7 but significantly more than the 46.6% lower central incisor intrusion accuracy reported by Kravitz and colleagues.8 The discrepancy could be attributable to the development of SmartTrack aligner material, which was not yet available for the study by Kravitz and colleagues. It could also be related to measurements being made in our sample from lateral cephalograms instead of virtual models created from pre- and post-treatment impressions.
Through their years of experience, the two clinicians involved with our study have learned to routinely build overcorrection into their ClinCheck prescriptions. Therefore, the cases analyzed might have finished ideally regardless of the lack of intrusion obtained relative to what was requested. The equation shown above provides a rough estimate of how much overcorrection should be requested in a ClinCheck. Further research is needed, however, as the equation was derived from a limited data set and becomes more inaccurate as larger amounts of intrusion are requested.
Our sizable standard deviation of .78mm indicates a wide variability in the differences between requested and obtained intrusion measurements. Of the 30 patients, nine showed a difference of .1mm or less, demonstrating nearly perfect tracking on a clinical level. Sixteen of the 30 had differences of less than .5mm, an amount that is likely to be of minimal clinical significance.
The CR of the traced lower incisor, as defined by Profitt and colleagues,11 was used as the reference point for evaluating true absolute intrusion, as proposed by Burstone15 and Kale Varlik and colleagues.16 Although this method was utilized in an effort to determine absolute incisor intrusion rather than relative intrusion, it has its limitations. We assumed that the intrusion of CR was independent of any change in the axial inclination of the incisor. There is a possibility that CR could move apically, however, due to proclination of the incisor. Although minimal, this relative intrusion would make the reported intrusion greater than the actual intrusion. CR is also poorly defined: several sources define it as the point approximately one-third to two-fifths, rather than one-half, of the distance from the alveolar crest to the apex of the tooth.15,17-19 Using a different definition for CR could provide results that show either more or less accuracy in the measurement of lower incisor intrusion.
This study also had limitations due to its lack of randomization and its retrospective design. Selection bias was still possible, even though consecutively treated patients were chosen from two orthodontists with extensive clear-aligner experience, without regard to treatment outcomes. The issue of patient compliance is still a major factor in evaluating the effectiveness of aligner therapy. While the patients were instructed to change aligners every two weeks, compliance was not accounted for in this study; the assumption was made that the compliance of the consecutively treated patients reflected those of a standard orthodontic practice. As aligner technology continues to develop and more treatment options—such as bite ramps fabricated into the aligners or customized rates of intrusion—become available, studies with larger sample sizes will be needed to refine our proposed equation and more accurately utilize clear aligners for lower incisor intrusion.
FOOTNOTES
- *Registered trademark of Align Technology, Inc., Santa Clara, CA; www.aligntech.com.
- **3M Unitek, Monrovia, CA; www.3MUnitek.com.
REFERENCES
- 1. Rosvall, M.D.; Fields, H.W.; Ziuchkovski, J.; Rosenstiel, S.F.; and Johnston, W.M.: Attractiveness, acceptability, and value of orthodontic appliances, Am. J. Orthod. 135:276e1-276e12, discussion 276-277, 2009.
- 2. Meier, B.; Wiemer, K.B.; and Miethke, R.R.: Invisalign—Patient profiling: Analysis of a prospective survey, J. Orofac. Orthop. 64:352-358, 2003.
- 3. Align Technology: Why Invisalign, www.invisalign.com/why-invisalign, accessed Dec. 8, 2016.
- 4. Buschang, P.H.; Shaw, S.G.; Ross, M.; Crosby, D.; and Campbell, P.M.: Comparative time efficiency of aligner therapy and conventional edgewise braces, Angle Orthod. 84:391-396, 2013.
- 5. Boyd, R.L. and Waskalic, V.: Three-dimensional diagnosis and orthodontic treatment of complex malocclusion with the Invisalign appliance, Semin. Orthod. 7:274-293, 2001.
- 6. Burstone, C.R.: Deep overbite correction by intrusion, Am. J. Orthod. 72:1-22, 1977.
- 7. Nguyen, C.V. and Cheng, J.: Three-dimensional superimposition tool, in The Invisalign System, ed. O.C. Tuncay, Quintessence Publishing Co., New Malden, U.K., 2006, pp. 12-32.
- 8. Kravitz, N.D.; Kusnoto, B.; BeGole, E.; Obrez, A.; and Agran, B.: How well does Invisalign work? A prospective clinical study evaluating the efficacy of tooth movement with Invisalign, Am. J. Orthod. 135:27-35, 2009.
- 9. Rossini, G.; Parrini, S.; Castroflorio, T.; Deregibus, A.; and Debernardi, C.L.: Efficacy of clear aligners in controlling orthodontic tooth movement: A systematic review, Angle Orthod. 85:881-889, 2015.
- 10. Align Technology: SmartTrack aligner material: Q&A, www.provider.invisalign.com/smarttrack_qa, accessed June 1, 2015.
- 11. Proffit, W.R.; Fields, H.W. Jr.; and Sarver, D.M.: Contemporary Orthodontics, Mosby/Elsevier, St. Louis, 2014, p. 324.
- 12. Bland, J.M. and Altman, D.G.: Statistical methods for assessing agreement between two methods of clinical measurement, Lancet 327:307-310, 1986.
- 13. Filippi, M.; Horsfield, M.A.; Rovaris, M.; Yousry, T.; Rocca, M.A.; Baratti, C.; Bressi, S.; and Comi, G.: Intraobserver and interobserver variability in schemes for estimating volume of brain lesions on MR images in multiple sclerosis, Am. J. Neuroradiol. 19:239-244, 1998.
- 14. Draper, N.R. and Smith, H.: Applied Regression Analysis, 3rd ed., John Wiley & Sons, New York, 1966, p. 24.
- 15. Burstone, C.J.: The biomechanics of tooth movement, in Vistas in Orthodontics, ed. B.S. Kraus and R.A. Riedel, Lea & Febiger, Philadelphia, 1962, pp. 197-213.
- 16. Kale Varlik, S.; Onur Alpakan, Ö.; and Türköz, Ç.: Deepbite correction with incisor intrusion in adults: A long-term cephalometric study, Am. J. Orthod. 144:414-419, 2013.
- 17. Department of Orthodontics, University of Illinois at Chicago: Glossary of commonly-used terms in orthodontics, www.uic.edu/depts/dort/glossary.html, accessed Sept. 1, 2015.
- 18. Hans, M.G.; Kishiyama, C.; Parker, S.H.; Wolf, G.R.; and Noachtar, R.: Cephalometric evaluation of two treatment strategies for deep overbite correction, Angle Orthod. 64:265-274, 1994.
- 19. Polat-Özsoy, Ö.; Arman-Özçırpıcı, A.; Veziroğlu, F.; and Çetinşahin, A.: Comparison of the intrusive effects of miniscrews and utility arches, Am. J. Orthod. 139:526-532, 2011.






