Corticotomy-Enhanced Intrusion of an Overerupted Molar Using Skeletal Anchorage and Ultrasonic Surgery
Overerupted molars due to the loss of antagonists are a common clinical finding in adults. Because intrusion of an overerupted molar to permit prosthetic replacement is difficult to achieve without adverse side effects on the neighboring teeth, skeletal anchorage is now commonly used.1-5
Several surgical techniques have been proposed to allow faster orthodontic movement in these cases. Wilcko and colleagues developed an accelerated osteogenic technique involving full-thickness flap reflection, selective alveolar decortication, ostectomy, and bone grafting.6 Other authors have recommended selective alveolar corticotomy involving full-thickness flaps and vertical and horizontal corticotomies limited to the cortical bone.7-9
Kim and colleagues proposed a minimally invasive technique called corticision to induce accelerated tooth movement by stimulating osteoblasts and bending the surgically separated alveolar bone.10 In this technique, a reinforced scalpel is used as a thin chisel to separate the interproximal cortices transmucosally without reflecting a flap. Vercellotti and Podesta recently introduced a new approach to bone surgery involving flap elevation and vertical and horizontal osteotomies performed with an ultrasonic piezosurgical device.11 Piezocision, an evolution of this technique developed by Dibart and colleagues,12,13 is a minimally invasive procedure that combines microincisions and localized piezoelectric surgery without flap elevation.
Similar articles from the archive:
In a previous article, we described the use of the Mectron Piezosurgery* unit (Fig. 1) for exposure of a palatally impacted canine.14 This device is a powerful piezoelectric handpiece with a functional frequency of 25-29kHz and a digital modulation capability of 30Hz. It improves surgical control by performing a precise, selective cut, using ultrasonic waves transmitted to the hard tissues through an insert mounted on the handpiece. The inserts vibrate linearly between 60 and 210 microns, providing the handpiece with power in excess of 5W. A high-powered pump emits a biocompatible .9% sodium chloride solution for cooling.
This article shows how intrusion of an overerupted molar with skeletal anchorage can be enhanced by selective alveolar corticotomy using ultrasonic bone surgery.
Case Report
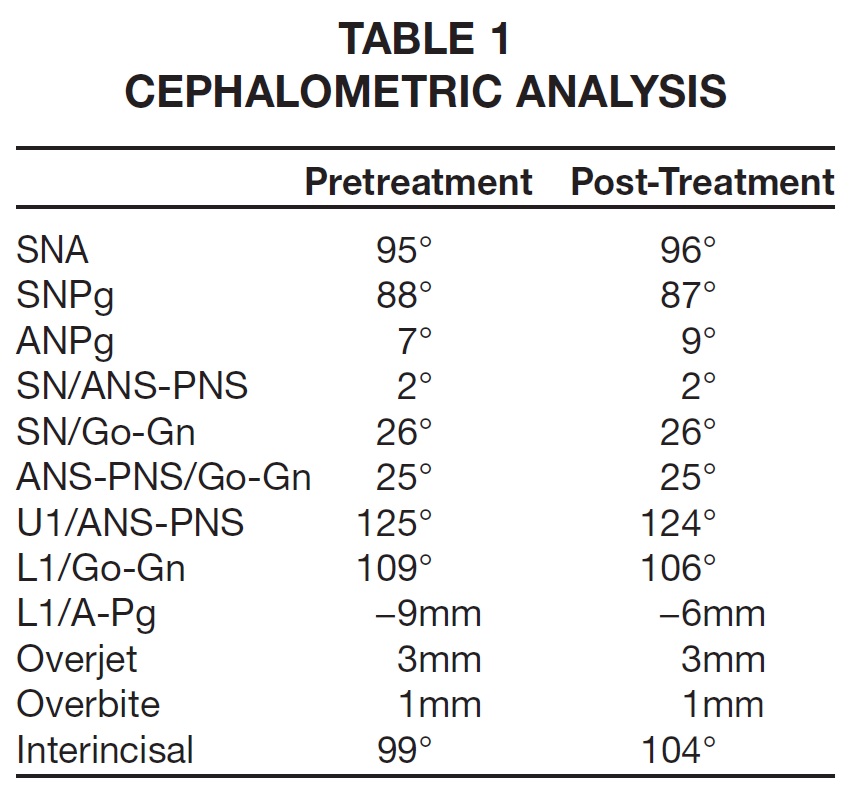
A 35-year-old male presented with the chief complaint of space between the upper central incisors; he also sought restoration of his posterior occlusion. Clinical analysis showed a Class I malocclusion with protrusion of the maxillary and mandibular incisors and a deviation of the maxillary midline to the right (Fig. 2, Table 1).
The upper right first premolar and second molar and left second premolar were missing, as well as the lower left first and second molars and right first molar. The panoramic radiograph revealed that the roots of the upper right first premolar, upper left second premolar, and lower left first molar were still present. Periodontal disease was evident throughout the entire dental field. The absence of lower molars had led to overeruption of both upper first molars, especially on the left side, but the patient showed no facial asymmetry or TMD. Cephalometric analysis verified skeletal protrusion of the maxilla and mandible, with normal vertical measurements.
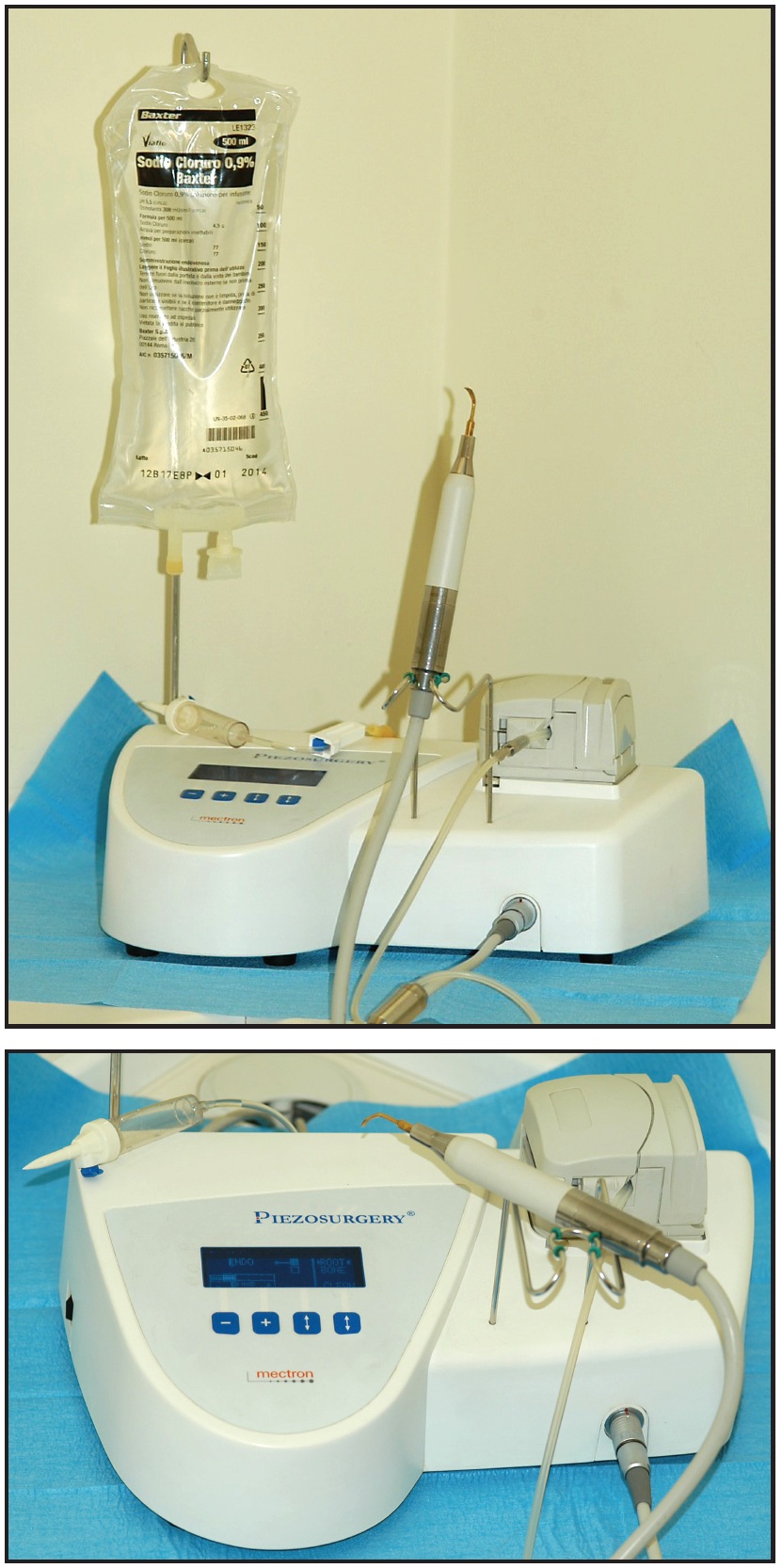
Fig. 1 Mectron Piezosurgery device.
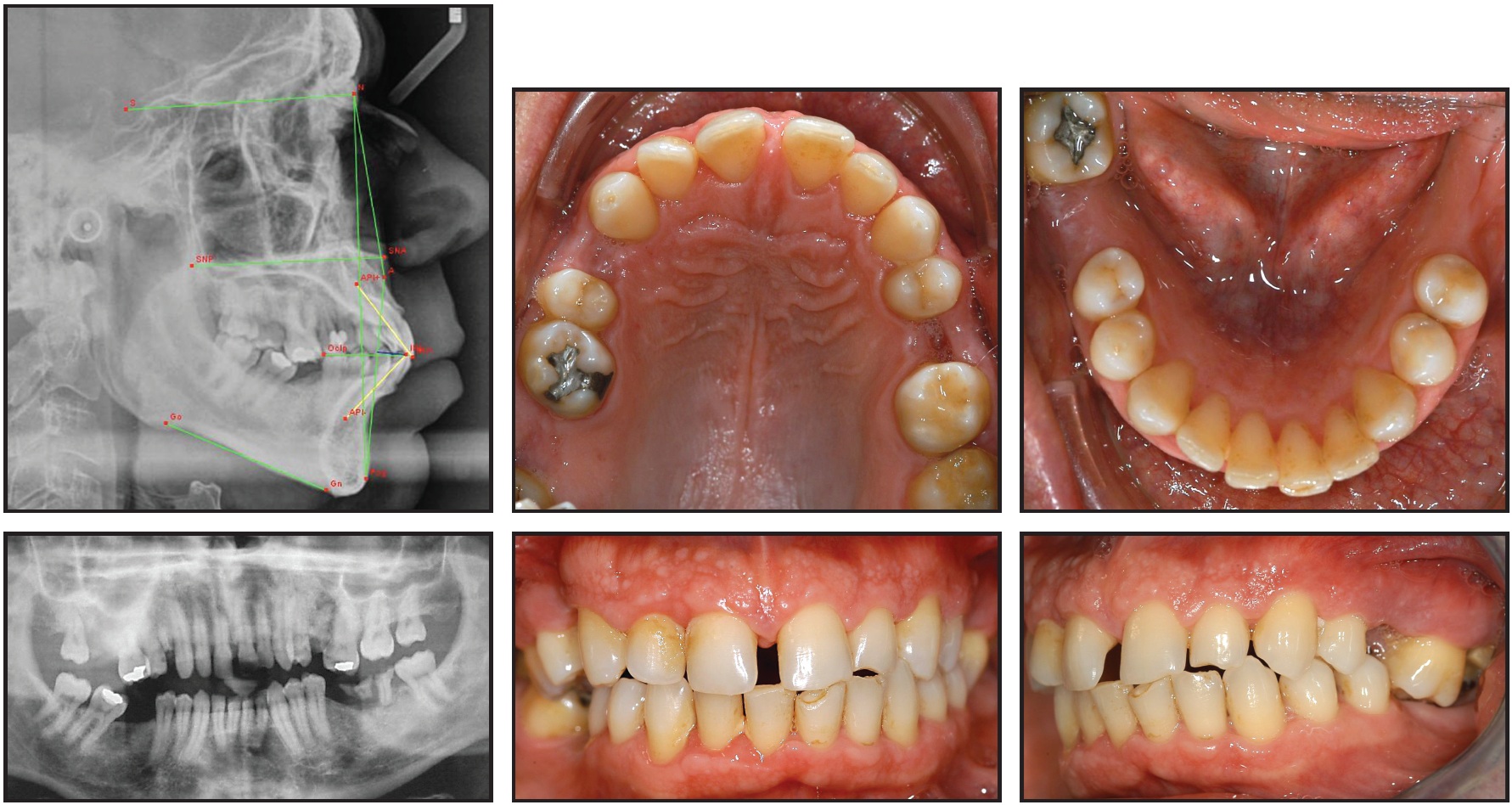
Fig. 2 35-year-old male patient with overerupted upper left first molar before treatment.
The treatment plan involved removal of the remnant premolar and molar roots and improvement of the patient's oral hygiene and periodontal status. Orthodontic treatment would align the upper and lower anterior teeth, close the midline space, and correct the midline deviation. In the posterior regions, preparation for future implants and prosthetic replacement of the missing premolars and molars would be accomplished through intrusion of the upper left first molar, uprighting of the lower left second molar, and intrusion and distalization of the upper right second premolar and first molar. Piezoelectric surgery followed by skeletally anchored intrusion was planned for the significantly overerupted upper left first molar.
After extraction of the premolar and molar roots and subgingival scaling and root planing in all four quadrants, orthodontic treatment began with leveling and alignment of the mandibular arch, followed by space closure and uprighting of the lower right second molar.
The surgical procedure for the upper left first molar was performed under local anesthesia (Fig. 3A). Mucogingival flaps were elevated on the palatal and buccal sides of the overerupted molar to expose the cortical bone completely beyond the apex (Fig. 3B). Vertical bone cuts were made with the ultrasonic device (insert OT7S) 1-2mm mesial and distal to the left first molar, extending to a point 1mm beyond the apex (Fig. 3C). Particular attention was paid to the inclination of the bone cuts to ensure the proper direction of molar intrusion. Two horizontal bone cuts were made above the apex of the first molar, and a small slice of cortical bone was removed to permit easier vertical movement of the tooth (Fig. 3D). The intact membrane of the maxillary sinus was evident after removal of the bone slice (Fig. 3E). A similar procedure was performed on the palatal side (Fig. 3F). Precise and selective surgery, with the depth of the bone cuts limited to the cortical bone, allowed the osteotomies to be performed without damaging the soft tissues.
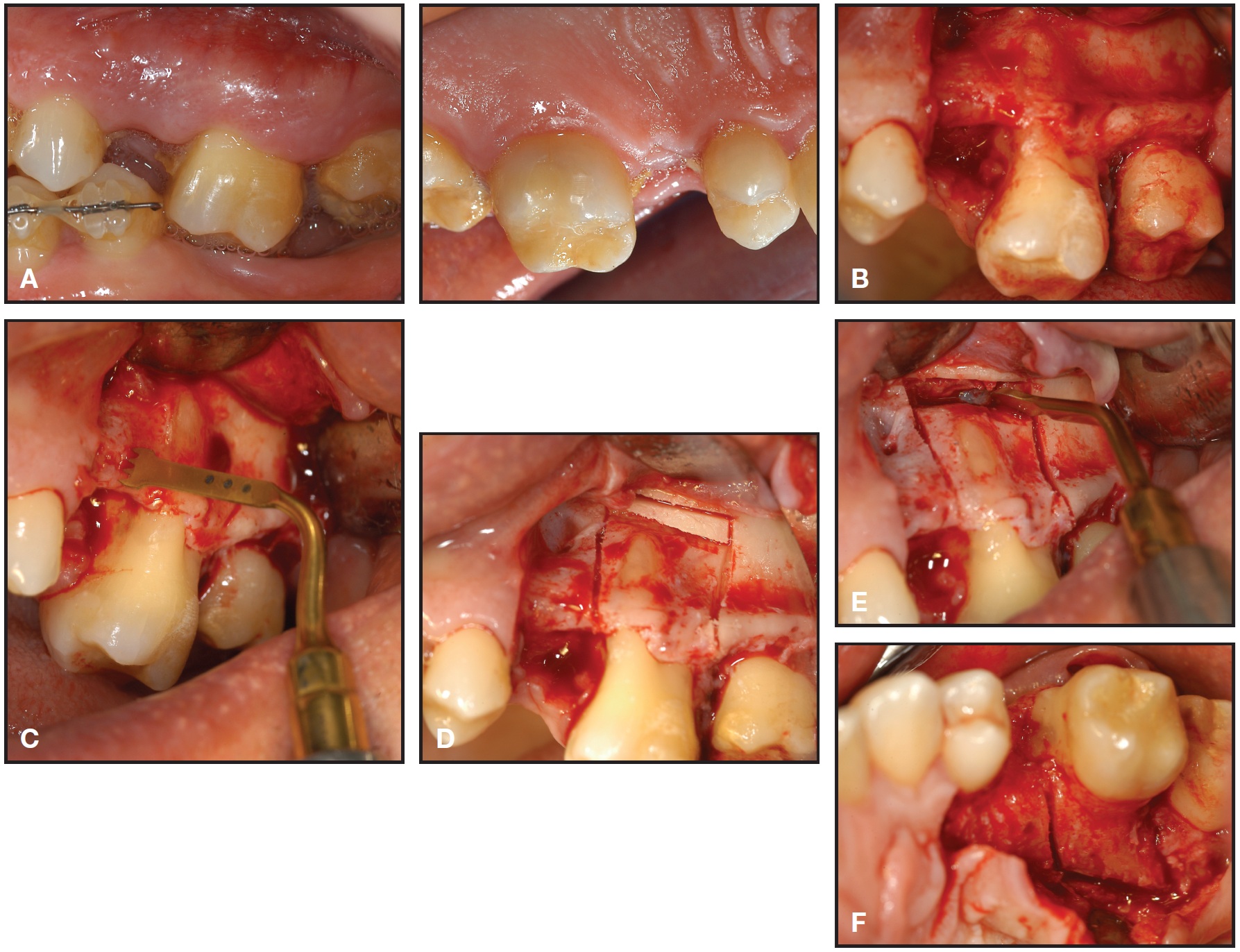
Fig. 3 A. Buccal and palatal views of upper left first molar area prior to surgery. B. Cortical bone exposed after flap elevation on buccal and palatal sides. C. Vertical bone cuts made with OT7S insert of piezoelectric device. D. Two horizontal bone cuts made on buccal aspect above first-molar apex; slice of cortical bone removed to permit easier vertical movement of molar. E. Intact membrane of maxillary sinus after removal of bone slice. F. Bone cuts made on palatal side.
To provide skeletal anchorage for the molar intrusion, two miniscrews were inserted on the buccal side, immediately mesial and distal to the vertical bone cuts, at the height of the apex of the upper first molar's vestibular roots. A third miniscrew was inserted on the palatal side, mesial to the mesial vertical bone cut, in the bone space of the absent left second premolar. The buccal and palatal flaps were then sutured.
Immediately after surgery, power chain was attached between the buccal screws and the bonded first-molar tube (Fig. 4A). On the palatal side, a ligature wire was tied between the miniscrew and a lingually bonded button as passive anchorage to prevent excessive buccal movement of the tooth during the first two months of intrusion (Fig. 4B). Moderate buccal tipping of the molar was desirable to correct a crossbite of the upper left first molar, probably caused by the extrusion.
Ten days after surgery, when the power chain was changed, initial molar intrusion was evident (Fig. 5A). After 30 days, the power chain was replaced with a nickel titanium coil spring that exerted a more continuous force on the tooth (Fig. 5B). After 60 days, a power chain was applied on both the buccal and palatal sides (Fig. 5C). Significant intrusion was achieved in four months (Fig. 5D); the mesial buccal miniscrew was then removed, and traction was maintained only on the distal screw to obtain distal movement of the tooth, opening space between the first premolar and first molar. Six months after surgery, the maxillary left first molar was completely level with the rest of the arch. The remaining screws were removed, and the maxillary arch was fully bonded (Fig. 5E).
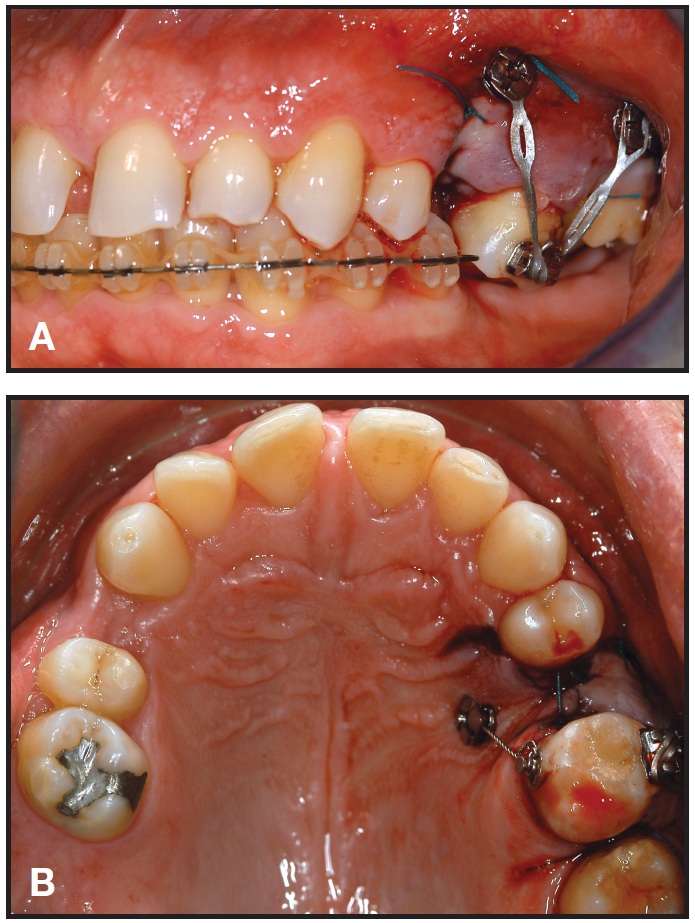
Fig. 4 A. Two buccal miniscrews inserted, mesial and distal to vertical bone cuts; power chain attached between buccal screws and molar tube. B. Palatal ligature wire applied as passive anchorage to avoid excessive vestibular molar movement during initial intrusion.
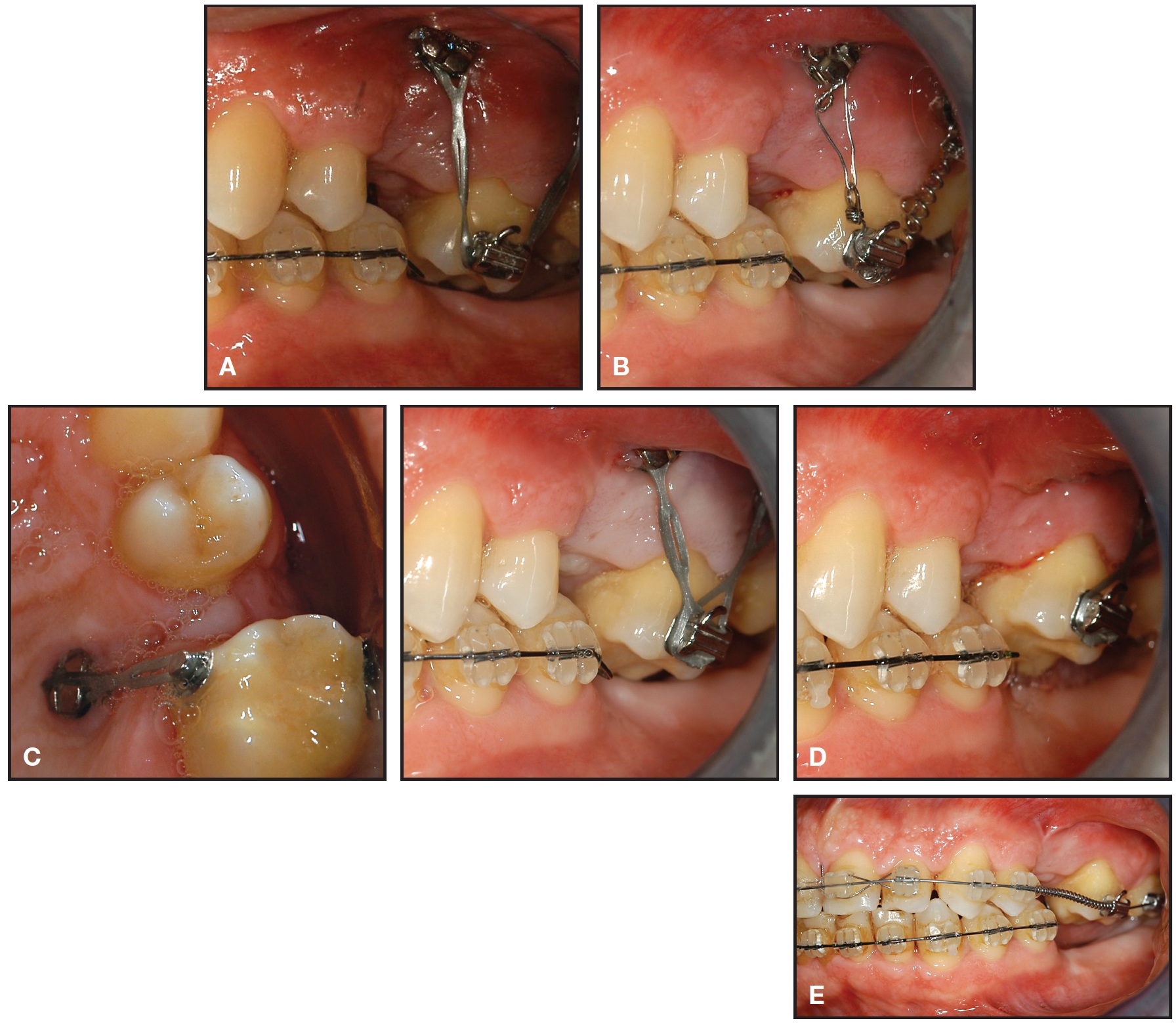
Fig. 5 A. Molar intrusion 10 days after surgery. B. 30 days after surgery, power chain replaced with nickel titanium coil spring to provide more continuous forces. C. Two months after surgery, power chain applied on both palatal and buccal sides. D. Significant intrusion four months after surgery; mesial buccal screw removed and traction maintained only on distal screw to open space between first molar and first premolar. E. Six months after surgery, upper left first molar completely level with maxillary arch; remaining screws removed and upper arch bonded.
Upper-arch alignment, leveling, and space management were completed over the next 12 months. Three dental implants were placed in the mandible and two in the maxilla, and final tooth movements were completed. After 20 months of orthodontic treatment, fixed appliances were removed, and ceramic crowns were placed over the five implants (Fig. 6). The post-treatment panoramic radiograph showed no root resorption and proper integration of the implants. Cephalometric analysis confirmed no significant change in the skeletal values and a slight improvement in the anterior dental values (Table 1)
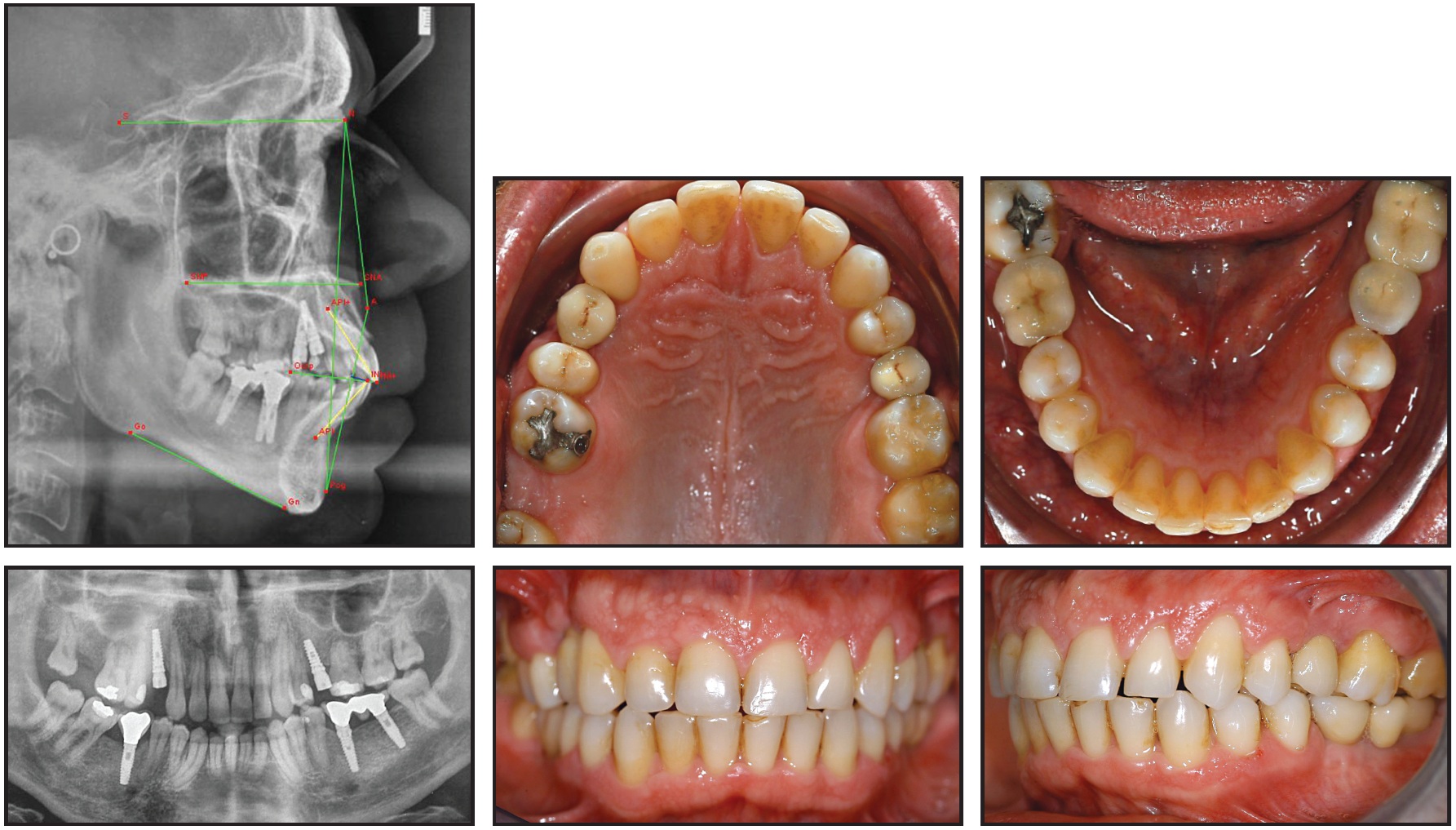
Fig. 6 Patient after 20 months of orthodontic treatment and prosthodontic replacement of five missing teeth.
The patient was happy with the outcome of his treatment and motivated to continue with better oral hygiene.
Conclusion
While overerupted molars can be effectively intruded without side effects using skeletal anchorage, corticotomy can assist in achieving the required intrusion in a shorter time with more predictable results. Ultrasonic piezoelectric surgery is safer and induces less bone trauma than other methods for performing the osteotomies.
FOOTNOTES
- *Registered trademark of Mectron Medical Technology, Carasco, Italy; www.mectron.com.
REFERENCES
- 1. Lin, J.C. and Liou, E.J.: A new bone screw for orthodontic anchorage, J. Clin. Orthod. 37:676-681, 2003
- 2. Block, S.M. and Hoffman, D.R.: A new device for absolute anchorage for orthodontics, Am. J. Orthod. 107:251-258, 1995.
- 3. Maino, B.G.; Bednar, J.; Pagin, P.; and Mura, P.: The Spider Screw for skeletal anchorage, J. Clin. Orthod. 37:90-97, 2003.
- 4. Kyung, H.M.; Park, H.S.; Bae, S.M.; Sung, J.H.; and Kim, I.B.: Development of orthodontic micro-implants for intraoral anchorage, J. Clin. Orthod. 37:321-328, 2003.
- 5. Costa, A.; Raffaini, M.; and Melsen, B.: Miniscrews as orthodontic anchorage: A preliminary report, Int. J. Adult Orthod. Orthog. Surg. 13:201-209, 1998.
- 6. Wilcko, M.T.; Wilcko, W.M.; Pulver, J.J.; Bissada, N.F.; and Bouquot, J.E.: Accelerated osteogenic orthodontics technique: A 1-stage surgically facilitated rapid orthodontic technique with alveolar augmentation, J. Oral Maxillofac. Surg. 67:2149-2159, 2009.
- 7. Moon, C.H. and Lee, H.S.: Intrusion of overerupted molars by corticotomy and orthodontic skeletal anchorage, Angle Orthod. 77:1119-1125, 2007.
- 8. Kim, S.H.; Kook, Y.A.; Jeong, D.M.; Lee, W.; Chung, K.R.; and Nelson, G.: Clinical application of accelerated osteogenic orthodontics and partially osseointegrated mini-implants for minor tooth movement, Am. J. Orthod. 136:431-439, 2009.
- 9. Oliveira, D.D.; De Oliveira, B.F.; De Araujo Brito, H.H.; Gomes De Souza, M.M.; and Medeiros, P.J.: Selective alveolar corticotomy to intrude overerupted molars, Am. J. Orthod. 133:902-908, 2008.
- 10. Kim, S.; Park, Y.; and Kang, S.: Effects of corticision on paradental remodeling in orthodontic tooth movement, Angle Orthod. 79:284-291, 2009.
- 11. Vercellotti, T. and Podesta, A.: Orthodontic microsurgery: A new surgically guided technique for dental movement, Int. J. Period. Restor. Dent. 27:325-331, 2007.
- 12. Dibart, S.; Sebaoun, J.D.; and Surmenian, J.: Piezocision: A minimally invasive, periodontally accelerated orthodontic tooth movement procedure, Compend. Cont. Ed. Dent. 30:342-350, 2009.
- 13. Dibart, S.; Surmenian, J.; Sebaoun, J.D.; and Montesani, L.: Rapid treatment of Class II malocclusion with piezocision: Two case reports, Int. J. Period. Restor. Dent. 30:487-493, 2010.
- 14. Grenga, V. and Bovi, M.: Piezoelectric surgery for exposure of palatally impacted canines, J. Clin. Orthod. 38:446-448, 2004.



